These statistics form part of the National Nutrition and Physical Activity Survey (NNPAS), which ran from January 2023 to March 2024. More information on other topics of interest from the survey are available on the NNPAS 2023 page.
Usual nutrient intakes
Provides a distributional analysis of usual nutrient consumption enabling population assessment of intakes against the Nutrient Reference Values
Key statistics
- Six in ten (63.7%) people did not meet their dietary calcium requirements
- Females were more likely to have an inadequate iron intake than males (26.8% compared to 8.2%)
- Nearly two in three (65.6%) adults had a usual sodium intake above the Suggested Dietary Target of 2,000 mg/day or less
- Children between 2 and 11 years generally had adequate intakes of most vitamins and minerals, except for calcium
About usual nutrient intakes
This second release of nutrition results from the NNPAS 2023 presents analysis on usual nutrient intakes as an estimate of what people eat and drink over the long-term. It complements the first Food and nutrients release, which reported on average food consumption and energy and nutrient intakes based on a single day only. The first release showed that, overall, energy intake decreased between 2011–12 and 2023, and intakes of most micronutrients have either decreased or remained stable.
Inadequate nutrient intakes can lead to chronic conditions, which often take weeks, months or years to develop[1]. Long-term (usual) intake of nutrients, and prevalence of inadequate intakes, can be modelled using multiple days of food consumption. This approach accounts for the day-to-day variation from a single day of dietary recall data[2].
Interpreting usual nutrient intakes
This analysis presents long-term (usual) nutrient intakes for each age and sex group using a combination of the following statistics:
- proportion of people whose usual nutrient intakes were inadequate or in excess
- median (and other percentiles) to describe the distribution of usual nutrient intakes across the population.
The average usual nutrient intake is often similar to the average intake for a single day (such as those presented in the Food and nutrients release). However, using multiple days of data provides a more accurate estimate of the distribution (or spread) of nutrient intakes and the proportion of people who are not consuming enough of each nutrient to meet their requirements.
Percentiles can be useful to demonstrate the shape of a distribution (or spread) of intakes for nutrients. For example, comparing the:
- 5th percentile to the median (50th percentile) illustrates how low intakes compare to the middle point
- 95th percentile to the median (50th percentile) illustrates how high intakes compare to the middle point.
This analysis does not include nutrient intake from dietary supplements, which will be the focus of a future release. See Dietary Supplements for information on people who reported consuming dietary supplements in 2023.
Like other nutrition surveys, it is likely there has been some under-reporting of food and beverage consumption by respondents in NNPAS 2023. This is unlikely to affect all foods and nutrients equally and readers should be aware of under-reporting while interpreting the results in this analysis. See methodology for more information.
Nutrient Reference Values
Nutrient Reference Values (NRVs) are a set of recommendations that describe the nutrient intake amounts required at different life stages to meet nutritional needs and reduce the risk of developing chronic conditions[1]. This analysis compares usual intakes of selected nutrients to the relevant NRVs for each age and sex group, including the:
- Acceptable Macronutrient Distribution Range (AMDR) – the range of percentage contributions to total energy from macronutrients that would allow for an adequate intake of all the other macro- and micronutrients while maximising general health outcomes
- Estimated Average Requirement (EAR) – the daily amount estimated to meet the nutrient intake requirements of half the healthy individuals in a particular age, sex and life stage group
- Upper Level of intake (UL) – the highest daily nutrient intake level likely to pose no adverse health effects to almost all individuals in the general population
- Suggested Dietary Target (SDT) – a daily average nutrient intake from food and beverages that may help in prevention of chronic conditions.
When usual nutrient intakes are close to the EAR or UL, it does not imply an adverse effect will occur. As intakes become more extreme (i.e. further below the EAR or further above the UL), then the risk of an adverse effect occurring will increase.
Weighted NRVs for each nutrient have been calculated using new reference age groups. See IHMHS: Concepts, Sources and Methods for more information.
Comparisons over time
This analysis uses the cut-point method to estimate the proportion of people whose usual nutrient intakes were below the relevant EAR (inadequate) or above the relevant UL (excess). Large changes in the proportion below the EAR or above the UL over time may occur even if there is only a small change in a population’s average usual intake.
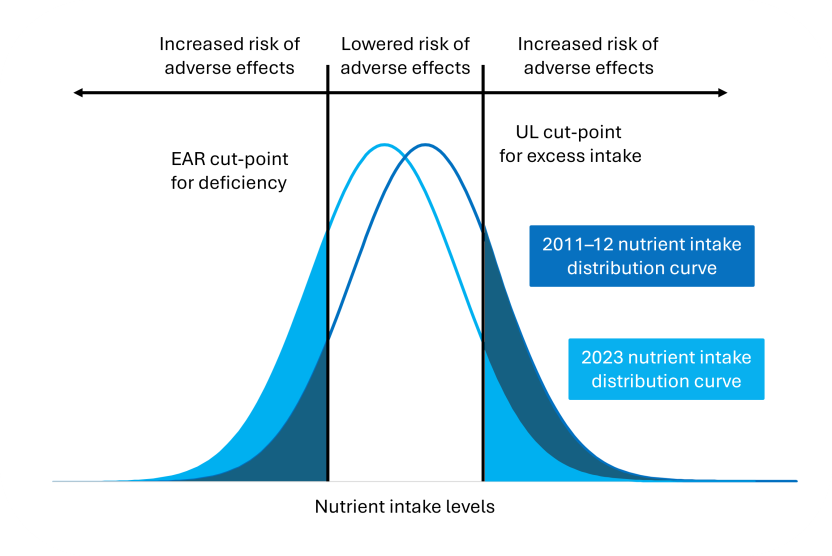
For example, a small decrease in usual intakes will shift the distribution of nutrient intakes towards to the left of the nutrient intake scale. If the average usual intake is also close to the EAR, then significantly more of the intake distribution may fall below the cut-point (see figure below and vitamins B6 and B12 for examples of this trend occurring over time).
Image
Description
Graph showing two normally distributed curves, one with slightly higher values (situated further to the right in dark blue).
A line to the left in the graph shows the “EAR cut-point for deficiency” and a line to the right shows the “UL cut-point for excess intake”. An additional line at the top of the graph illustrates that when intake is between the two cut-points, there is a lowered risk of adverse effects. When intake is above the UL or below the EAR, there is an increased risk of adverse effects.
Both the EAR and UL cut-point lines are cutting off different proportions of the curves, indicating that when a small decrease in usual intakes shifts the distribution to the left of the nutrient scale, significantly more of the distribution may fall below/above the cut-point.
See IHMHS: Concepts, Sources and Methods for more information on the use of NRVs to measure the proportion of people with an inadequate or excess nutrient intake.
AUSNUT food groups
The ABS collected two days of dietary information from respondents aged 2 years and over through a 24-hour dietary recall tool called Intake24. Food and drinks reported as consumed by respondents were then classified according to the AUSNUT (AUStralian Food and NUTrient Database) 2023 food and dietary supplement classification developed by Food Standards Australia New Zealand.
Information about how energy and nutrient intakes were derived from the foods and beverages that respondents reported consuming can be found in the Food and nutrients release.
Sub-major AUSNUT food groups that have contributed to nutrient intake are discussed in this analysis and some of these names have been abbreviated for ease of reading. These are outlined in the following table.
| Sub-major food group code | AUSNUT 2023 sub-major food group name | Abbreviated name |
|---|---|---|
| 118 | Water (municipal and bottled) | Water |
| 121 | Flours, rice and other cereal grains and starches | Flours, rice and other cereal grains |
| 122 | Regular breads, and bread rolls (plain, unfilled and untopped varieties) | Bread and bread rolls |
| 125 | Breakfast cereals, ready to eat | Ready to eat breakfast cereals |
| 135 | Mixed dishes where cereal is the major ingredient | Cereal-based mixed dishes |
| 187 | Mixed dishes where beef, sheep, pork or mammalian game is the major component | Beef, sheep and pork-based mixed dishes |
| 189 | Mixed dishes where poultry or feathered game is the major component | Poultry-based mixed dishes |
| 191 | Dairy milk (cow, sheep and goat) | Dairy milk |
| 249 | Dishes where vegetable is the major component | Vegetable-based mixed dishes |
Macronutrients
Macronutrients are the components of food that contribute to energy intake and are needed by the body in large amounts to function properly. They primarily include carbohydrates, proteins, and fats. Small amounts of energy also come from alcohol and dietary fibre[1].
Acceptable Macronutrient Distribution Ranges (AMDR)
The risk of developing chronic conditions increases as imbalances among relative proportions of macronutrients increase. AMDRs specify the proportion of energy from each macronutrient that is recommended to reduce this risk[1]. As the AMDR acts as a ratio, an increase in the proportional contribution to energy for one macronutrient means a decrease in one, or more, of the other macronutrients.
In 2023, the average usual proportion of energy intake from carbohydrate was below the AMDR for both males and females. The proportion of energy from fat and protein were within their respective AMDRs.
| Macronutrient | AMDR (%) | Proportion of energy intake (%) | |
|---|---|---|---|
| Males | Females | ||
| Carbohydrate | 45–65 | 43 | 43 |
| Fat | 20–35 | 32 | 33 |
| Protein | 15–25 | 19 | 19 |
- AMDRs are published in Australia by the National Health and Medical Research Council in the Nutrient Reference Values for Australia and New Zealand.
This analysis also estimates the proportion of the population whose macronutrient balance was outside the AMDRs. The proportion of people whose contribution to energy from carbohydrate was:
- lower than the AMDR was 57.8%
- higher than the AMDR was less than 5%.
The proportion of people whose contribution to energy from fat was:
- lower than the AMDR was less than 5%
- higher than the AMDR was 25.2%.
The proportion of people whose contribution to energy from protein was:
- lower than the AMDR was 11.9%
- higher than the AMDR was 5.3%.
Proportion of people with usual proportion of energy intake from macronutrients below, within or above the AMDR(a), by age, 2023
["Macronutrient","Age group","Proportion"]
[{"name":"Carbohydrate, below AMDR","value":"57.8","data":[{"name":"Children aged 2\u201317 years","value":"23"},{"name":"Adults aged 18 years and over","value":"66.9"}]},{"name":"Carbohydrate, within AMDR","value":"42.2","data":[{"name":"Children aged 2\u201317 years","value":"77"},{"name":"Adults aged 18 years and over","value":"33.1"}]},{"name":"Carbohydrate, above AMDR(b)","value":"0","data":[{"name":"Children aged 2\u201317 years(b)","value":"0"},{"name":"Adults aged 18 years and over(b)","value":"0"}]},{"name":"Fat, below AMDR(b)","value":"0.1","data":[{"name":"Children aged 2\u201317 years(b)","value":"0"},{"name":"Adults aged 18 years and over(b)","value":"0.1"}]},{"name":"Fat, within AMDR","value":"74.7","data":[{"name":"Children aged 2\u201317 years","value":"81.8"},{"name":"Adults aged 18 years and over","value":"72.9"}]},{"name":"Fat, above AMDR","value":"25.2","data":[{"name":"Children aged 2\u201317 years","value":"18.2"},{"name":"Adults aged 18 years and over","value":"27"}]},{"name":"Protein, below AMDR","value":"11.9","data":[{"name":"Children aged 2\u201317 years","value":"26.2"},{"name":"Adults aged 18 years and over","value":"8.2"}]},{"name":"Protein, within AMDR","value":"82.8","data":[{"name":"Children aged 2\u201317 years","value":"72.8"},{"name":"Adults aged 18 years and over","value":"85.3"}]},{"name":"Protein, above AMDR","value":"5.3","data":[{"name":"Children aged 2\u201317 years","value":"1"},{"name":"Adults aged 18 years and over","value":"6.5"}]}][]
[{"value":"0","axis_id":"0","axis_title":"Macronutrients","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- Acceptable Macronutrient Distribution Range. AMDR are published in Australia by the National Health and Medical Research Council in the Nutrient Reference Values for Australia and New Zealand.
- This proportion has a high margin of error and should be used with caution.
The balance of usual proportion of energy intake from macronutrients has changed between 2011–12 and 2023. The proportion of people with energy from:
- carbohydrate lower than the AMDR has increased from 50.2% to 57.8%
- fat higher than the AMDR has increased from 14.4% to 25.2%
- protein higher than the AMDR has increased from 1.5% to 5.3%
- protein lower than the AMDR has decreased from 16.6% to 11.9%.
| Below AMDR (%) | Within AMDR (%) | Above AMDR (%) | |
|---|---|---|---|
| Carbohydrate, 2011–12 | 50.2 | 49.7 | 0.1 |
| Carbohydrate, 2023 | 57.8 | 42.2 | 0.0 |
| Fat, 2011–12 | 0.3 | 85.3 | 14.4 |
| Fat, 2023 | 0.1 | 74.7 | 25.2 |
| Protein, 2011–12 | 16.6 | 81.9 | 1.5 |
| Protein, 2023 | 11.9 | 82.8 | 5.3 |
Proportion of people 2 years and over with usual proportion of energy intake from macronutrients below, within or above the AMDR(a), 2011–12 and 2023
["","Below AMDR","Within AMDR","Above AMDR"]
[["Carbohydrate, 2011\u201312","Carbohydrate, 2023","Fat, 2011\u201312","Fat, 2023","Protein, 2011\u201312","Protein, 2023"],[[50.2],[57.8],[0.3],[0.1],[16.6],[11.9]],[[49.7],[42.2],[85.3],[74.7],[81.9],[82.8]],[[0.1],[0],[14.4],[25.2],[1.5],[5.3]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Macronutrients","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- Acceptable Macronutrient Distribution Range. AMDR are published in Australia by the National Health and Medical Research Council in the Nutrient Reference Values for Australia and New Zealand.
The increase in the usual proportion of energy from fat and protein over time is likely a result of an overall decrease in daily energy from reduced carbohydrate intakes. This balance is explored in the Food and nutrients release in more detail.
Carbohydrate
Carbohydrates are an important major source of energy for the body, particularly the brain. The two major types of carbohydrates are sugars and starch. Nearly one-third (32.1%) of dietary carbohydrate in 2023 came from:
- Cereal-based mixed dishes (like sandwiches and pasta/noodle dishes)
- Bread and bread rolls
- Flours, rice and other cereal grains.
Between 2011–12 and 2023, the average usual carbohydrate intake decreased for:
- males aged 2 years and over (259 g/day compared to 237 g/day)
- females aged 2 years and over (198 g/day compared to 187 g/day).
See the AMDR section above for analysis on the proportion of energy intake from carbohydrate in the diet.
Sugars
Sugar intakes are part of the total carbohydrate intakes. Free sugars include all the added sugars put into foods during their processing or preparation as well as the sugars that are naturally present in fruit and vegetable juice, syrups and honey. Sugars naturally present in unrefined foods, such as whole fruit or unflavoured milk, are not considered free sugars but are included in total sugar intakes[3].
In 2023, the average usual intake of total sugars was:
- 91 g/day for males
- 76 g/day for females.
High intakes of sugar can lead to increased risk of chronic conditions such as heart disease, stroke, and some forms of cancer[4]. Among males, the 95th percentile of usual intake of total sugars was:
- 163 g/day, equivalent to three and a half cans of cola soft drink
- almost two times higher than the median (86 g/day).
Similarly, the 95th percentile of usual intake of total sugars for females was:
- 131 g/day, equivalent to two and a half cans of cola soft drink
- almost two times higher than the median (72 g/day).
The average usual intake of total sugars decreased for males and females in almost all age groups between 2011–12 and 2023, except among females aged 75 years and over where the difference was not statistically significant (88 g/day and 82 g/day).
Following the same pattern as total sugars, males had higher average usual intake than females of:
- free sugars (49 g/day compared to 39 g/day)
- added sugars (43 g/day compared to 33 g/day).
More detailed analysis on free and added sugars will be included in a future release.
Protein
Protein supports normal tissue maintenance and growth. Proteins consumed in the diet are broken down by the body to make new proteins or to be used as a source of energy[1]. Inadequate intakes of protein can lead to weakness, anaemia, and protein energy undernutrition[1][5]. One-third of (34.5%) of dietary protein in 2023 came from:
- Cereal-based mixed dishes (including pasta/noodle dishes and sandwiches)
- Beef, sheep and pork, unprocessed
- Poultry and feathered game.
Almost all (98.5%) people had an adequate protein intake in 2023, which was slightly lower than 2011–12 (99.1%). People aged 75 years and over have the highest protein requirements and were more likely to have an inadequate protein intake than any other age group (14.7% for males and 6.2% for females).
| Male EAR (g/day) | Female EAR (g/day) | Males (%) | Females (%) | |
|---|---|---|---|---|
| 2–4(a) | 13 | 13 | 0 | 0 |
| 5–11(a) | 22 | 19 | 0 | 0 |
| 12–17(a) | 43 | 31 | 0.1 | 0.1 |
| 18–29(a) | 52 | 37 | 0.7 | 0.5 |
| 30–49(b) | 52 | 37 | 0.8 | 0.3 |
| 50–64(b) | 52 | 37 | 1.3 | 0.5 |
| 65–74 | 57 | 41 | 5.1 | 1.7 |
| 75 years and over | 65 | 46 | 14.7 | 6.2 |
Proportion of people with an inadequate protein intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","Male EAR","Female EAR","Males","Females"]
[["2\u20134(a)","5\u201311(a)","12\u201317(a)","18\u201329(a)","30\u201349(b)","50\u201364(b)","65\u201374","75 years and over"],[[13],[22],[43],[52],[52],[52],[57],[65]],[[13],[19],[31],[37],[37],[37],[41],[46]],[[0],[0],[0.1],[0.7],[0.8],[1.3],[5.1],[14.7]],[[0],[0],[0.1],[0.5],[0.3],[0.5],[1.7],[6.2]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Grams per day (g\/day)","axis_units":"","tooltip_units":"(g\/day)","table_units":"(g\/day)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportions for ‘Males’ and ‘Females’ have high margins of error and should be used with caution.
- The proportion for ‘Females’ has a high margin of error and should be used with caution.
The 95th percentile of protein intake for:
- males was 53 g/day higher than the median (151 g/day or more compared to 98 g/day), equivalent to almost one medium size grilled beef steak
- females was 35 g/day higher than the median (110 g/day or more compared to 75 g/day), equivalent to one and a third cups of ricotta cheese.
Although both an AMDR and EAR apply to protein, the results are interpreted differently. It is possible to have a sufficient intake of protein while having a low contribution to energy from protein, relative to other macronutrients, which can lead to an increased risk of chronic disease. Although most people met their protein requirements, over one in ten (11.9%) were not getting enough energy from protein relative to the other macronutrients they consumed.
See the AMDR section above for analysis on the proportion of energy intake from protein in the diet.
Fat
Fat has the highest energy density of the macronutrients. In addition to being a concentrated form of energy, fats help the body absorb fat-soluble vitamins, such as vitamin A. Diets high in fat can increase the risk of heart attack and stroke[4]. One-quarter (26.7%) of dietary fat in 2023 came from:
- Cereal-based mixed dishes (like pizza and pasta/noodle dishes)
- Poultry-based mixed dishes
- Potatoes and potato products and dishes.
The average usual fat intake in 2023 was higher for males than for females (81 g/day compared to 65 g/day). For males, the average usual fat intake was:
- lowest for children aged 2–4 years and 5–11 years
- highest overall for children aged 12–17 years
- higher for adults aged between 18 and 64 years than for adults aged 65 years and over.
The average usual fat intake for females was:
- lowest for children aged 2–4 years and adults aged 75 years and over
- generally similar for females in age groups between 5 and 64 years.
| Males (g/day) | 95% confidence interval (g/day) (low) | 95% confidence interval (g/day) (high) | Females (g/day) | 95% confidence interval (g/day) (low) | 95% confidence interval (g/day) (high) | |
|---|---|---|---|---|---|---|
| 2–4 | 52.7 | 49.3 | 56.1 | 47.3 | 44.6 | 50.0 |
| 5–11 | 70.0 | 66.7 | 73.3 | 63.5 | 60.8 | 66.2 |
| 12–17 | 93.6 | 88.1 | 99.1 | 69.9 | 65.1 | 74.7 |
| 18–29 | 85.5 | 80.5 | 90.5 | 64.6 | 61.3 | 67.9 |
| 30–49 | 83.2 | 80.4 | 86.0 | 67.1 | 64.2 | 70.0 |
| 50–64 | 82.0 | 78.6 | 85.4 | 64.8 | 61.8 | 67.8 |
| 65–74 | 75.0 | 71.3 | 78.7 | 65.1 | 61.8 | 68.4 |
| 75 years and over | 75.2 | 71.2 | 79.2 | 59.3 | 56.2 | 62.4 |
Average usual intake of fat, by age and sex, 2023
["","Males","95% confidence interval","Females","95% confidence interval"]
[["2\u20134","5\u201311","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[52.7],[70],[93.6],[85.5],[83.2],[82],[75],[75.2]],[[49.3,56.1],[66.7,73.3],[88.1,99.1],[80.5,90.5],[80.4,86],[78.6,85.4],[71.3,78.7],[71.2,79.2]],[[47.3],[63.5],[69.9],[64.6],[67.1],[64.8],[65.1],[59.3]],[[44.6,50],[60.8,66.2],[65.1,74.7],[61.3,67.9],[64.2,70],[61.8,67.8],[61.8,68.4],[56.2,62.4]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"Grams per day (g\/day)","axis_units":"","tooltip_units":"(g\/day)","table_units":"(g\/day)","axis_min":null,"axis_max":"100","tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]Males aged 12–17 years had the highest average usual fat intake (94 g/day) when compared to other age groups. Among males aged 12–17 years:
- 10% had a usual fat intake of less than 61 g/day (10th percentile), equivalent to 4 tablespoons of butter or less
- 10% had a usual fat intake of more than 128 g/day (90th percentile), equivalent to 8 tablespoons of butter or more.
Between 2011–12 and 2023, the average usual fat intake has remained similar across most age and sex groups but has:
- decreased for males aged 30–49 years (87 g/day compared to 83 g/day)
- increased for females aged 65–74 years (59 g/day compared to 65 g/day).
See the AMDR section above for analysis on the proportion of energy intake from fat in the diet.
Alcohol
Pure alcohol is a relatively high source of energy, second only to fat in energy density. Consumption of alcohol can be harmful to health and no level can be guaranteed as completely safe. Alcohol intake as a nutrient refers to pure alcohol (ethanol) and intake estimates are calculated from alcoholic drinks or other foods that contain small amounts (e.g. soy sauce). There is no NRV for alcohol, however it is generally recommended that it should account for less than 5% of energy intake[1]. For information on the consumption of Alcoholic beverages as a food group, see Food and beverage consumption.
In 2023, the average usual alcohol intake (expressed as pure ethanol) for adults was:
- higher for males than for females (10 g/day compared to 7 g/day)
- higher for males in every age group than females
- lowest among females aged 18–29 years (3 g/day) than any other adult age group, regardless of sex.
The average usual contribution to energy intake from alcohol was the same between adult males and females (at 3%).
The proportion of adults who had a usual contribution to energy intake from alcohol that was below 5% was:
- higher for females than males (85.2% compared to 80.1%)
- higher for males aged 18–29 years (90.7%) than other male adult age groups
- higher for females aged 18–29 years (94.3%) than other female adult age groups.
| Males (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | Females (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | |
|---|---|---|---|---|---|---|
| 18–29 | 90.7 | 87.2 | 94.2 | 94.3 | 91.0 | 97.6 |
| 30–49 | 84.1 | 80.5 | 87.7 | 86.3 | 83.3 | 89.3 |
| 50–64 | 74.3 | 69.8 | 78.8 | 78.9 | 74.4 | 83.4 |
| 65–74 | 66.6 | 60.9 | 72.3 | 80.4 | 75.9 | 84.9 |
| 75 years and over | 71.2 | 64.6 | 77.8 | 86.0 | 81.5 | 90.5 |
Proportion of adults with a usual contribution to energy intake from alcohol of less than 5%, by age and sex, 2023
["","Males","95% confidence interval","Females","95% confidence interval"]
[["18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[90.7],[84.1],[74.3],[66.6],[71.2]],[[87.2,94.2],[80.5,87.7],[69.8,78.8],[60.9,72.3],[64.6,77.8]],[[94.3],[86.3],[78.9],[80.4],[86]],[[91,97.6],[83.3,89.3],[74.4,83.4],[75.9,84.9],[81.5,90.5]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":"100","tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]The average usual contribution to energy intake from alcohol has decreased over the last decade for most adult age groups, except for males 75 years and over and for females 50 years and over where the differences were not statistically significant.
| Males, 2011–12 (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | Males, 2023 (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | Females, 2011–12 (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | Females, 2023 (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 18–29 | 3 | 2 | 4 | 2 | 1 | 3 | 2 | 1 | 3 | 1 | 1 | 1 |
| 30–49 | 5 | 5 | 5 | 3 | 3 | 3 | 4 | 4 | 4 | 2 | 2 | 2 |
| 50–64 | 7 | 6 | 8 | 4 | 3 | 5 | 5 | 4 | 6 | 4 | 3 | 5 |
| 65–74 | 7 | 6 | 8 | 5 | 4 | 6 | 4 | 3 | 5 | 3 | 2 | 4 |
| 75 years and over | 5 | 4 | 6 | 4 | 3 | 5 | 3 | 2 | 4 | 2 | 1 | 3 |
Average usual contribution to energy intake from alcohol for adults, by age and sex, 2011–12 and 2023
["","Males, 2011\u201312","95% confidence interval","Males, 2023","95% confidence interval","Females, 2011\u201312","95% confidence interval","Females, 2023","95% confidence interval"]
[["18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[3],[5],[7],[7],[5]],[[2,4],[5,5],[6,8],[6,8],[4,6]],[[2],[3],[4],[5],[4]],[[1,3],[3,3],[3,5],[4,6],[3,5]],[[2],[4],[5],[4],[3]],[[1,3],[4,4],[4,6],[3,5],[2,4]],[[1],[2],[4],[3],[2]],[[1,1],[2,2],[3,5],[2,4],[1,3]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]Vitamins
Vitamins ensure the proper functioning of the body, including normal cell function, immune function, growth and development. Vitamins are needed in small amounts and are obtained through a varied diet as the body is unable to make most of them on its own, except for vitamin D. Deficiencies can lead to severe health conditions and increase the risk of other conditions[6].
Between 2011–12 and 2023, the proportion of people with an inadequate intake from food and beverages:
- increased for almost all vitamins (except for niacin equivalents)
- remained low (less than 10% for all vitamins) for children under 12 years.
More information on prevalence of inadequate vitamin intakes from food and beverages for each sex and age group is detailed below. These results do not consider the contribution of dietary supplements to intake.
This analysis does not focus on the group average for usual vitamin intakes, which is available in Table 5 from the Data downloads. Average nutrient intake based on a single day of intake is explored in more detail in the Food and nutrients release.
Vitamin A
Vitamin A helps with normal immune function, vision, and reproduction. Deficiencies can lead to difficulty adjusting to low light and night blindness[1]. Around two-fifths (39.5%) of dietary vitamin A (as retinol equivalents) in 2023 came from:
- Carrot and similar root vegetables
- Cereal-based mixed dishes (which include sandwiches and pasta/noodle dishes)
- Vegetable-based mixed dishes.
Over one in five (22.9% or 5.7 million) people aged 2 years and over had an inadequate vitamin A intake from food and beverages in 2023. The proportion was:
- lower for children aged 2–17 years than adults aged 18 years and over (14.8% and 25.0%)
- among children, similar between males and females (13.7% and 16.0%)
- among adults, higher for males than females (29.8% compared to 20.2%).
| Male EAR (µg/day) | Female EAR (µg/day) | Males (%) | Females (%) | |
|---|---|---|---|---|
| 2–4(a) | 230 | 230 | 2.1 | 4.0 |
| 5–11 | 350 | 335 | 7.4 | 10.4 |
| 12–17 | 570 | 465 | 26.8 | 28.5 |
| 18–29 | 625 | 500 | 42.9 | 27.2 |
| 30–49 | 625 | 500 | 28.7 | 19.2 |
| 50–64 | 625 | 500 | 24.2 | 21.7 |
| 65–74 | 625 | 500 | 25.7 | 13.3 |
| 75 years and over | 625 | 500 | 22.2 | 15.9 |
Proportion of people with an inadequate vitamin A intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","Male EAR","Female EAR","Males","Females"]
[["2\u20134(a)","5\u201311","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[230],[350],[570],[625],[625],[625],[625],[625]],[[230],[335],[465],[500],[500],[500],[500],[500]],[[2.1],[7.4],[26.8],[42.9],[28.7],[24.2],[25.7],[22.2]],[[4],[10.4],[28.5],[27.2],[19.2],[21.7],[13.3],[15.9]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Micrograms per day (\u00b5g\/day)","axis_units":"","tooltip_units":"(\u00b5g\/day)","table_units":"(\u00b5g\/day)","axis_min":"0","axis_max":null,"tick_interval":null,"precision":"0","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportions for 'Males' and 'Females' have high margins of error and should be used with caution.
Four in ten (42.9%) males aged 18–29 years had an inadequate vitamin A intake, which was higher than any other adult male age group despite having the same requirements. Analysis of the distribution of vitamin A intake shows that the value of most percentiles were lower in this group than other adult male age groups, indicating a lower overall intake.
The proportion of people with an inadequate vitamin A intake has increased from 15.5% in 2011–12 to 22.9% in 2023. This was primarily due to increases among:
- adult males aged 18 years and over (up from 18.3% to 29.8%)
- females aged 50–64 years (up from 11.8% to 21.7%).
For these groups, the distribution of vitamin A intake has shifted to the left with a lower average usual intake in 2023 when compared to 2011–12, contributing to the increased proportion of people who did not meet their requirements.
The UL for vitamin A refers to preformed vitamin A (retinol). Less than 5% of the population exceeded the UL for preformed vitamin A, a pattern which has remained unchanged since 2011–12.
These results do not consider the contribution of dietary supplements to vitamin A intake. Nutrient intake from supplements will be included in a future Dietary supplements release.
Thiamin (vitamin B1)
Thiamin (vitamin B1) helps the body convert food into energy for the brain, nervous system and muscles. Deficiencies can increase the risk of chronic conditions with compromised cardiac function or neurological damage[1]. Wheat flour for bread making is fortified with thiamin in Australia to reduce the risk of developing deficiencies[7]. Almost half (46.2%) of dietary thiamin in 2023 came from:
- Cereal-based mixed dishes (such as sandwiches and pizza)
- Bread and bread rolls
- Yeast extracts (such as spreads like Vegemite).
Over one in six (15.5% or 3.8 million) people aged 2 years and over had an inadequate thiamin intake from food and beverages in 2023. The proportion was:
- less than 5% for children aged 2–4 and 5–11 years
- higher for females than males in all adult age groups
- similar across all adult male age groups (ranging from 10.9% to 14.3%)
- similar across all adult female age groups (ranging from 20.4% to 28.9%).
| Male EAR (mg/day) | Female EAR (mg/day) | Males (%) | Females (%) | |
|---|---|---|---|---|
| 2–4(a) | 0.4 | 0.4 | 0.1 | 0.4 |
| 5–11(a) | 0.6 | 0.6 | 0.3 | 1.0 |
| 12–17 | 0.9 | 0.8 | 3.3 | 7.2 |
| 18–29 | 1.0 | 0.9 | 13.6 | 28.9 |
| 30–49 | 1.0 | 0.9 | 14.3 | 23.4 |
| 50–64 | 1.0 | 0.9 | 11.4 | 27.1 |
| 65–74 | 1.0 | 0.9 | 12.3 | 23.0 |
| 75 years and over | 1.0 | 0.9 | 10.9 | 20.4 |
Proportion of people with an inadequate thiamin intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","Male EAR","Female EAR","Males","Females"]
[["2\u20134(a)","5\u201311(a)","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[0.4],[0.6],[0.9],[1],[1],[1],[1],[1]],[[0.4],[0.6],[0.8],[0.9],[0.9],[0.9],[0.9],[0.9]],[[0.1],[0.3],[3.3],[13.6],[14.3],[11.4],[12.3],[10.9]],[[0.4],[1],[7.2],[28.9],[23.4],[27.1],[23],[20.4]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":"40","tick_interval":"10","precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Milligrams per day (mg\/day)","axis_units":"","tooltip_units":"(mg\/day)","table_units":"(mg\/day)","axis_min":"0","axis_max":null,"tick_interval":"0.2","precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportions for 'Males' and 'Females' have high margins of error and should be used with caution.
The proportion of adults with an inadequate thiamin intake was higher for females than males even though males have higher requirements to account for differences in body size and energy needs[1]. This reflects the lower usual average and percentiles of intake among females when compared to males.
The proportion of people with an inadequate thiamin intake increased slightly from 11.1% in 2011–12 to 15.5% in 2023. This was primarily due to increases among:
- adult males (8.3% to 12.9%)
- adult females (19.0% to 24.9%).
For adults, the distribution of thiamin intake had shifted to the left with a lower average usual intake in 2023 than in 2011–12, contributing to an increase in the proportion of adults with an inadequate intake.
These results do not consider the contribution of dietary supplements to thiamin intake. Nutrient intake from supplements will be included in a future Dietary supplements release.
Riboflavin (vitamin B2)
Riboflavin (vitamin B2) is important for converting other nutrients into forms that can be used by the body. Deficiencies can lead to delayed growth, skin rashes and inflammation of the tongue. Nearly one third (32.9%) of dietary riboflavin in 2023 came from:
- Dairy milk
- Ready to eat breakfast cereals
- Cereal-based mixed dishes (such as sandwiches and pizza).
One in five (19.7% or 4.9 million) people aged 2 years and over had an inadequate riboflavin intake from food and beverages in 2023. The proportion was:
- lower for children than for adults (6.4% compared to 23.2%)
- among adults, similar between males and females (21.8% and 24.6%).
| Male EAR (mg/day) | Female EAR (mg/day) | Males (%) | Females (%) | |
|---|---|---|---|---|
| 2–4(a)(b) | 0.4 | 0.4 | 0.1 | 0.5 |
| 5–11(b) | 0.6 | 0.6 | 0.7 | 2.7 |
| 12–17 | 1.0 | 0.9 | 8.2 | 22.3 |
| 18–29 | 1.1 | 0.9 | 22.3 | 27.1 |
| 30–49 | 1.1 | 0.9 | 21.2 | 24.3 |
| 50–64 | 1.1 | 0.9 | 18.8 | 22.5 |
| 65–74 | 1.2 | 1.0 | 25.2 | 24.7 |
| 75 years and over | 1.3 | 1.1 | 25.8 | 26.0 |
Proportion of people with an inadequate riboflavin intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","Male EAR","Female EAR","Males","Females"]
[["2\u20134(a)(b)","5\u201311(b)","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[0.4],[0.6],[1],[1.1],[1.1],[1.1],[1.2],[1.3]],[[0.4],[0.6],[0.9],[0.9],[0.9],[0.9],[1],[1.1]],[[0.1],[0.7],[8.2],[22.3],[21.2],[18.8],[25.2],[25.8]],[[0.5],[2.7],[22.3],[27.1],[24.3],[22.5],[24.7],[26]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":"30","tick_interval":"10","precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Milligrams per day (mg\/day)","axis_units":"","tooltip_units":"(mg\/day)","table_units":"(mg\/day)","axis_min":"0","axis_max":null,"tick_interval":"0.2","precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportion for 'Males' has a high margin of error and should be used with caution.
- The proportion for 'Females' has a high margin of error and should be used with caution.
The proportion of children with an inadequate riboflavin intake was higher for females than males (9.7% compared to 3.4%). Additionally, of people aged 12–17 years, females:
- were more likely to have an inadequate riboflavin intake (22.3% compared to 8.2% for males)
- had a lower average usual riboflavin intake (1.3 mg/day compared to 1.9 mg/day for males)
- had a distribution of usual riboflavin intakes that was further to the left than males.
The proportion of adults with an inadequate riboflavin intake was similar across all:
- male adult age groups (ranging between 18.8% and 25.8%)
- female adult age groups (ranging between 22.5% and 27.1%).
People aged 65–74 years and 75 years and over were similarly likely to have an inadequate riboflavin intake as younger adult age groups even though their requirements are higher because of age effects on absorption and metabolism[1].
The proportion of people aged 2 years and over with an inadequate riboflavin intake increased from 6.9% in 2011–12 to 19.7% in 2023. The proportion has increased for most age groups, but has remained similar among:
- children between 2 and 11 years
- males and females aged 75 years and over.
| Males | Females | |
|---|---|---|
| 2–4(a)(b) | 0.1 | 0.5 |
| 5–11(a) | 0.7 | 2.6 |
| 12–17 | 5.8 | 15.0 |
| 18–29 | 19.0 | 19.2 |
| 30–49 | 16.9 | 16.7 |
| 50–64 | 10.7 | 13.8 |
| 65–74 | 10.7 | 11.4 |
| 75 years and over(a)(b) | 5.6 | 6.3 |
Change in proportion of people with an inadequate riboflavin intake, by age and sex, 2011–12 and 2023
["","Males","Females"]
[["2\u20134(a)(b)","5\u201311(a)","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over(a)(b)"],[[0.1],[0.7],[5.8],[19],[16.9],[10.7],[10.7],[5.6]],[[0.5],[2.6],[15],[19.2],[16.7],[13.8],[11.4],[6.3]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"Percentage point change (%)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":"20","tick_interval":"5","precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The apparent difference between 2011–12 and 2023 for ‘Males’ is not statistically significant.
- The apparent difference between 2011–12 and 2023 for ‘Females’ is not statistically significant.
The distribution of riboflavin intake has shifted to the left with a lower average usual intake in 2023 when compared to 2011–12, except for people aged 75 years and over where intakes were similar. This reflects the increased proportion of people in most age groups who did not meet their requirements while the proportion was stable for those aged 75 years and over and children aged 2–4 and 5–11 years.
These results do not consider the contribution of dietary supplements to riboflavin intake. Nutrient intake from supplements will be included in a future Dietary supplements release.
Niacin (vitamin B3)
Niacin is involved in energy metabolism in the body and is found in a wide range of foods. Deficiencies are rare in Australia but can lead to inflammation of the skin on exposure to sunlight[1]. Over one third (35.8%) of dietary niacin (as niacin equivalents) in 2023 came from:
- Cereal-based mixed dishes (such as sandwiches and pasta/noodle dishes)
- Poultry and feathered game
- Poultry-based mixed dishes.
In 2023, the average usual niacin equivalents intake was 43 mg/day for males and 32 mg/day for females.
The proportion of people with an inadequate intake of niacin equivalents from food and beverages in 2023 was negligible (less than 5% for all age and sex groups).
The UL for niacin refers to nicotinic acid. This is a chemical form of niacin that was not reported separately in the NNPAS 2023, so the proportion of people with a usual intake of niacin in excess of the UL cannot be determined.
These results do not consider the contribution of dietary supplements to niacin intake. Nutrient intake from supplements will be included in a future Dietary supplements release.
Vitamin B6
Vitamin B6 helps with the metabolism of protein, carbohydrates, and fat, and helps in the formation of red blood cells. It is found in a wide range of foods and can also be sourced from dietary supplements. Deficiencies can lead to dermatitis, anaemia and convulsions[1]. Nearly one third (32.9%) of dietary vitamin B6 in 2023 came from:
- Electrolyte, energy and fortified drinks
- Cereal-based mixed dishes (such as sandwiches and pasta/noodle dishes)
- Poultry and feathered game.
High doses of vitamin B6 can lead to adverse side effects, including peripheral neuropathy. This usually occurs following long-term use of medicines containing vitamin B6 and is not associated with normal dietary intake levels[8]. These results do not consider the contribution of dietary supplements to vitamin B6 intake.
Almost one in two (46.7% or 11.5 million) people aged 2 years and over had an inadequate vitamin B6 intake from food and beverages in 2023. The proportion of people with an inadequate vitamin B6 intake was:
- higher for females than males (59.1% compared to 34.6%)
- higher for adults aged 18 years and over than children aged 2–17 years (54.9% compared to 15.3%)
- lower for adults aged 18–29 years and 30–49 years than adults in age groups over 50 years.
| Male EAR (mg/day) | Female EAR (mg/day) | Males (%) | Females (%) | |
|---|---|---|---|---|
| 2–4(a) | 0.4 | 0.4 | 2.3 | 4.2 |
| 5–11 | 0.6 | 0.6 | 5.3 | 9.1 |
| 12–17 | 1.0 | 0.9 | 19.1 | 42.9 |
| 18–29 | 1.1 | 1.1 | 25.7 | 58.7 |
| 30–49 | 1.1 | 1.1 | 27.6 | 60.2 |
| 50–64 | 1.4 | 1.3 | 56.9 | 77.7 |
| 65–74 | 1.4 | 1.3 | 62.1 | 80.2 |
| 75 years and over | 1.4 | 1.3 | 65.0 | 80.0 |
Proportion of people with an inadequate vitamin B6 intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","Male EAR","Female EAR","Males","Females"]
[["2\u20134(a)","5\u201311","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[0.4],[0.6],[1],[1.1],[1.1],[1.4],[1.4],[1.4]],[[0.4],[0.6],[0.9],[1.1],[1.1],[1.3],[1.3],[1.3]],[[2.3],[5.3],[19.1],[25.7],[27.6],[56.9],[62.1],[65]],[[4.2],[9.1],[42.9],[58.7],[60.2],[77.7],[80.2],[80]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Milligrams per day (mg\/day)","axis_units":"","tooltip_units":"(mg\/day)","table_units":"(mg\/day)","axis_min":null,"axis_max":null,"tick_interval":"0.2","precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportions for 'Males' and 'Females' have high margins of error and should be used with caution.
Around eight in ten (between 77.7% and 80.2%) females aged 50 years and over had an inadequate vitamin B6 intake from food and beverages in 2023. These groups have higher requirements than other female age groups and half of females in these age groups had a usual vitamin B6 intake that was at least 25% below (or around 0.4 mg/day) their vitamin B6 requirements.
The 5th percentile of vitamin B6 intake (lower end of the distribution) for all age and sex groups was less than 0.9 mg/day lower than the requirement for each age group (ranging from 0.4 mg/day to 1.4 mg/day).
Among people between 18 and 49 years, females were more likely to have an inadequate vitamin B6 intake than males despite having the same requirements:
- 18–29 years (58.7% for females compared to 25.7% for males)
- 30–49 years (60.2% for females compared to 27.6% for males).
Intakes for these male age groups were higher across each percentile of the usual vitamin B6 intake distribution than females, indicating an overall lower intake of vitamin B6 among females.
Between 2011–12 and 2023, the proportion of people with an inadequate vitamin B6 intake from food and beverages has:
- increased overall for people aged 2 years and over (from 28.9% to 46.7%)
- increased for all adult age groups, except among people aged 75 years and over where the difference was not significant.
| Males (%) | Females (%) | |
|---|---|---|
| 2–4(a)(b) | 2.3 | 3.8 |
| 5–11(b) | 4.4 | 5.5 |
| 12–17(a) | 5.0 | 13.2 |
| 18–29 | 20.9 | 23.5 |
| 30–49 | 19.4 | 22.2 |
| 50–64 | 20.5 | 20.1 |
| 65–74 | 16.8 | 16.1 |
| 75 years and over(a)(b) | 8.0 | 8.7 |
Change in proportion of people with an inadequate vitamin B6 intake, by age and sex, 2011–12 and 2023
["","Males","Females"]
[["2\u20134(a)(b)","5\u201311(b)","12\u201317(a)","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over(a)(b)"],[[2.3],[4.4],[5],[20.9],[19.4],[20.5],[16.8],[8]],[[3.8],[5.5],[13.2],[23.5],[22.2],[20.1],[16.1],[8.7]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"Percentage point change (%)","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":"5","precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The apparent difference between 2011–12 and 2023 for ‘Males’ is not statistically significant.
- The apparent difference between 2011–12 and 2023 for ‘Females’ is not statistically significant.
Analysis of the distribution of vitamin B6 intakes shows that over the past decade for adults aged 18 years and over, usual intakes for at least 75% of the population have decreased.
The absolute change in the distributions of vitamin B6 usual intake between 2011–12 and 2023 was small (ranging between 0.1 mg/day and 0.3 mg/day across each percentile). The small reduction in intake has meant that a much higher proportion of adults had an inadequate vitamin B6 intake in 2023 than did in 2011–12.
For more information on how small changes in the usual intake distribution can lead to large changes in proportions of people with inadequate nutrient intakes, see ‘Comparisons over Time’ in About usual nutrient intakes above.
These results do not consider the contribution of dietary supplements to vitamin B6 intake. Nutrient intake from supplements will be included in a future Dietary supplements release.
Folate (vitamin B9)
Folate is a B group vitamin (B9) that the body uses to make DNA and other genetic material. It is essential for healthy growth and development, particularly for the foetus in the first 3 months of pregnancy. Mandatory fortification of bread making flour with folic acid, a stable form of folate used in supplements and fortification, has been in place in Australia since 2009 to reduce the risk of folate deficiencies and the associated incidence of neural tube defects in babies[9]. Over half (54.0%) of dietary folate equivalents (DFE) in 2023 came from:
- Cereal-based mixed dishes (such as sandwiches and burgers)
- Bread and bread rolls
- Ready to eat breakfast cereals.
Less than one in ten (8.1% or 2.0 million) people aged 2 years and over had an inadequate DFE intake from food and beverages in 2023. The proportion was:
- less than 5% among male and female children
- among adults, higher for females than males (13.8% compared to 5.8%).
| EAR(c) (µg/day) | Males (%) | Females (%) | |
|---|---|---|---|
| 2–4(a) | 135 | 0.0 | 0.0 |
| 5–11(a) | 200 | 0.0 | 0.1 |
| 12–17(b) | 305 | 1.4 | 6.5 |
| 18–29 | 320 | 7.2 | 18.9 |
| 30–49 | 320 | 6.9 | 14.4 |
| 50–64 | 320 | 4.5 | 13.5 |
| 65–74 | 320 | 4.7 | 11.0 |
| 75 years and over | 320 | 3.2 | 7.6 |
Proportion of people with an inadequate DFE intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","EAR(c)","Males","Females"]
[["2\u20134(a)","5\u201311(a)","12\u201317(b)","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[135],[200],[305],[320],[320],[320],[320],[320]],[[0],[0],[1.4],[7.2],[6.9],[4.5],[4.7],[3.2]],[[0],[0.1],[6.5],[18.9],[14.4],[13.5],[11],[7.6]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Micrograms per day (\u00b5g\/day)","axis_units":"","tooltip_units":"(\u00b5g\/day)","table_units":"(\u00b5g\/day)","axis_min":"0","axis_max":null,"tick_interval":null,"precision":"0","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportions for 'Males' and 'Females' have high margins of error and should be used with caution.
- The proportion for 'Males' has a high margin of error and should be used with caution.
- EAR is the same for males and females in each age group.
Almost one in five (18.9%) females aged 18–29 years had an inadequate DFE intake, which was higher than older adult females aged 65–74 years (11.0%) and 75 years and over (7.6%) despite having the same requirements. The distribution of usual DFE intake was further to the left for females aged 18–29 years when compared to older female adult age groups, contributing to a lower average usual intake and a higher proportion with an inadequate intake.
The proportion of people with an inadequate DFE intake increased slightly from 4.8% in 2011–12 to 8.1% in 2023. This was primarily due to increases among:
- males aged 18–29 years (2.6% to 7.2%)
- males aged 30–49 years (2.5% to 6.9%)
- females aged 18–29 years (10.5% to 18.9%).
The UL for DFE refers to folic acid. Less than 5% of the population exceeded the UL for folic acid, a pattern which has remained unchanged since 2011–12.
These results do not consider the contribution of dietary supplements to folate intake. Nutrient intake from supplements will be included in a future Dietary supplements release.
Vitamin B12
Vitamin B12 is important for several functions in the body. It helps keep the body’s nerve and blood cells healthy and helps to make DNA. If left untreated, vitamin B12 deficiency can lead to anaemia, nerve damage and brain damage[1]. Almost all vitamin B12 comes from animal products. Over one third (34.5%) of dietary vitamin B12 in 2023 came from:
- Cereal-based mixed dishes (such as sandwiches and pasta/noodle dishes)
- Dairy milk
- Beef, sheep and pork, unprocessed.
One in ten (9.7% or 2.4 million) people aged 2 years and over had an inadequate vitamin B12 intake from food and beverages in 2023. The proportion of people with an inadequate vitamin B12 intake:
- was higher for females than males (13.9% compared to 5.6%)
- ranged between 5.4% and 9.0% for adult male age groups
- ranged between 11.6% and 19.1% for adult female age groups.
| EAR(c) (µg/day) | Males (%) | Females (%) | |
|---|---|---|---|
| 2–4(a)(b) | 0.80 | 0.2 | 0.8 |
| 5–11(a) | 1.20 | 0.7 | 2.5 |
| 12–17 | 1.80 | 3.9 | 13.6 |
| 18–29 | 2.00 | 5.4 | 19.1 |
| 30–49 | 2.00 | 5.9 | 15.9 |
| 50–64 | 2.00 | 7.2 | 17.0 |
| 65–74 | 2.00 | 9.0 | 11.8 |
| 75 years and over | 2.00 | 8.4 | 11.6 |
Proportion of people with an inadequate vitamin B12 intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","EAR(c)","Males","Females"]
[["2\u20134(a)(b)","5\u201311(a)","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[0.8],[1.2],[1.8],[2],[2],[2],[2],[2]],[[0.2],[0.7],[3.9],[5.4],[5.9],[7.2],[9],[8.4]],[[0.8],[2.5],[13.6],[19.1],[15.9],[17],[11.8],[11.6]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Micrograms per day (\u00b5g\/day)","axis_units":"","tooltip_units":"(\u00b5g\/day)","table_units":"(\u00b5g\/day)","axis_min":"0","axis_max":null,"tick_interval":null,"precision":"2","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportion for 'Males' has a high margin of error and should be used with caution.
- The proportion for 'Females' has a high margin of error and should be used with caution.
- EAR is the same for males and females in each age group.
Among people aged 18 to 64 years, females were more likely to have an inadequate vitamin B12 intake than males despite having the same requirements:
- 18–29 years (19.1% for females compared to 5.4% for males)
- 30–49 years (15.9% for females compared to 5.9% for males)
- 50–64 years (17.0% for females compared to 7.2% for males).
Intakes for these male age groups were higher across each percentile of the usual vitamin B12 intake distribution than females, indicating an overall lower intake of vitamin B12 among females.
The 5th percentile of vitamin B12 intakes (lower end of the distribution) for all adult age and sex groups in 2023 was less than 30% (or less than 0.6 µg/day) lower than their requirement (2.0 µg/day).
The proportion of people with an inadequate vitamin B12 intake from food and beverages increased from 2.8% in 2011–12 to 9.7% in 2023. There was an increase in every age and sex group except for children aged under 12 years. The proportion of adult females with an inadequate vitamin B12 intake increased particularly among the following age groups:
- 18–29 years (from 8.5% to 19.1%)
- 30–49 years (from 5.5% to 15.9%)
- 50–64 years (from 5.8% to 17.0%).
| Males (%) | Females (%) | |
|---|---|---|
| 2–4(a) | 0.2 | 0.8 |
| 5–11(a) | 0.6 | 2.2 |
| 12–17 | 3.8 | 8.2 |
| 18–29 | 5.4 | 10.6 |
| 30–49 | 5.8 | 10.4 |
| 50–64 | 6.9 | 11.2 |
| 65–74 | 8.4 | 5.7 |
| 75 years and over | 7.7 | 6.2 |
Change in proportion of people with an inadequate vitamin B12 intake, by age and sex, 2011–12 and 2023
["","Males","Females"]
[["2\u20134(a)","5\u201311(a)","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[0.2],[0.6],[3.8],[5.4],[5.8],[6.9],[8.4],[7.7]],[[0.8],[2.2],[8.2],[10.6],[10.4],[11.2],[5.7],[6.2]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"Percentage point change (%)","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":"2","precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The apparent difference between 2011–12 and 2023 for ‘Males’ and 'Females' is not statistically significant.
The increase in the proportion of people with an inadequate vitamin B12 intake reflects a shift of the usual intake distribution to the left. The decreases in the absolute value of the percentiles of vitamin B12 intake for all female and most male age groups over this period were 1.5 µg/day or less.
| EAR (µg/day) | 25th percentile (µg/day) | 50th percentile (median) (µg/day) | 75th percentile (µg/day) | |
|---|---|---|---|---|
| Males, 2011–12 | 2.0 | 4.1 | 5.1 | 6.1 |
| Males, 2023 | 2.0 | 2.9 | 3.9 | 5.1 |
| Females, 2011–12 | 2.0 | 2.8 | 3.6 | 4.6 |
| Females, 2023 | 2.0 | 2.3 | 3.0 | 3.8 |
Distribution of vitamin B12 intakes by sex, people aged 18 years and over, 2011–12 and 2023
["","EAR","25th percentile","50th percentile (median)","75th percentile"]
[["Males, 2011\u201312","Males, 2023","Females, 2011\u201312","Females, 2023"],[[2],[2],[2],[2]],[[4.1],[2.9],[2.8],[2.3]],[[5.1],[3.9],[3.6],[3]],[[6.1],[5.1],[4.6],[3.8]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Sex","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"Micrograms per day (\u00b5g\/day)","axis_units":"","tooltip_units":"(\u00b5g\/day)","table_units":"(\u00b5g\/day)","axis_min":"0","axis_max":"7","tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Micrograms per day (\u00b5g\/day)","axis_units":"","tooltip_units":"(\u00b5g\/day)","table_units":"(\u00b5g\/day)","axis_min":"0","axis_max":"7","tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]These results do not consider the contribution of dietary supplements to vitamin B12 intake. Nutrient intake from supplements will be included in a future Dietary supplements release.
Vitamin C
Vitamin C is an antioxidant and supports a range of metabolic processes. Deficiencies can cause scurvy with symptoms including gingivitis, oedema, ulcers and a tendency to bruise or bleed easily[1]. Nearly half (46.7%) of dietary vitamin C in 2023 came from:
- 100% Fruit and vegetable juices or Fruit and vegetable drinks
- Vegetable-based mixed dishes
- Cereal-based mixed dishes (such as rice-based dishes and sandwiches).
Less than one in ten (8.2% or 2.0 million) people aged 2 years and over had an inadequate vitamin C intake from food and beverages in 2023. The proportion was:
- similar between males and females (9.2% and 7.1%)
- higher among adults than children (9.0% compared to 5.1%)
- similar across most adult male age groups (ranging between 6.2% and 11.7%)
- similar across all adult female age groups (ranging between 6.7% and 9.3%).
| EAR(b) (mg/day) | Males (%) | Females (%) | |
|---|---|---|---|
| 2–4(a) | 25 | 5.3 | 4.3 |
| 5–11 | 26 | 3.9 | 3.5 |
| 12–17 | 28 | 8.3 | 5.7 |
| 18–29 | 30 | 11.6 | 9.3 |
| 30–49 | 30 | 11.7 | 7.4 |
| 50–64 | 30 | 9.1 | 8.1 |
| 65–74 | 30 | 7.8 | 6.7 |
| 75 years and over | 30 | 6.2 | 7.1 |
Proportion of people with an inadequate vitamin C intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","EAR(b)","Males","Females"]
[["2\u20134(a)","5\u201311","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[25],[26],[28],[30],[30],[30],[30],[30]],[[5.3],[3.9],[8.3],[11.6],[11.7],[9.1],[7.8],[6.2]],[[4.3],[3.5],[5.7],[9.3],[7.4],[8.1],[6.7],[7.1]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Milligrams per day (mg\/day)","axis_units":"","tooltip_units":"(mg\/day)","table_units":"(mg\/day)","axis_min":"0","axis_max":null,"tick_interval":null,"precision":"0","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportions for 'Males' and ‘Females’ have high margins of error and should be used with caution.
- EAR is the same for males and females in each age group.
The proportion of people with an inadequate vitamin C intake increased from 2.5% in 2011–12 to 8.2% in 2023. This proportion increased for all male and female age groups, except among children aged under 12 years, and females aged 12–17 years and 75 years and over where the differences were not significant.
| Males (%) | Females (%) | |
|---|---|---|
| 2–4(a)(b) | 2 | 0.3 |
| 5–11(a)(b) | 2.7 | 2 |
| 12–17(b) | 5.9 | 3.9 |
| 18–29 | 10 | 5.5 |
| 30–49 | 9.9 | 3.4 |
| 50–64 | 7.7 | 5.5 |
| 65–74 | 6.7 | 4.2 |
| 75 years and over(b) | 4.3 | 2.5 |
Change in proportion of people with an inadequate vitamin C intake, by age and sex, 2011–12 and 2023
["","Males","Females"]
[["2\u20134(a)(b)","5\u201311(a)(b)","12\u201317(b)","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over(b)"],[[2],[2.7],[5.9],[10],[9.9],[7.7],[6.7],[4.3]],[[0.3],[2],[3.9],[5.5],[3.4],[5.5],[4.2],[2.5]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"Percentage point change (%)","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":"12","tick_interval":"2","precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The apparent difference between 2011–12 and 2023 for ‘Males’ is not statistically significant.
- The apparent difference between 2011–12 and 2023 for ‘Females’ is not statistically significant.
The increase in the proportion of people with an inadequate vitamin C intake reflects the change to the distribution of usual vitamin C intake, which has shifted to the left in 2023 when compared to 2011–12.
These results do not consider the contribution of dietary supplements to vitamin C intake. Nutrient intake from supplements will be included in a future Dietary supplements release.
Vitamin D
Vitamin D is a hormone that helps the body to absorb and retain calcium and phosphorus. Deficiencies can lead to rickets in children and osteoporosis in adults[1]. Over one-third (35.9%) of dietary vitamin D (as vitamin D3 equivalents) in 2023 came from:
- Cereal-based mixed dishes (like sandwiches and pasta/noodle dishes)
- Eggs
- Poultry and feathered game.
There is no EAR for vitamin D intake from foods and beverages as vitamin D is mainly sourced from exposure to sunlight[1]. Previous results from the National Health Measures Survey 2022–24 reported that one in five (20.6%) of adults aged 18 years and over had a vitamin D deficiency.
Excess vitamin D intake may lead to hypercalcaemia (or increased serum calcium levels) which can further result in symptoms like increased urination and muscle weakness[1][10]. The proportion of people with a usual vitamin D intake above the UL was less than 5% for all age and sex groups in 2023.
These results do not consider the contribution of dietary supplements to vitamin D intake. Nutrient intake from supplements will be included in a future Dietary supplements release.
Essential minerals and caffeine
Essential minerals are required for a very wide variety of functions in the body including cell function, muscle function, bone formation, hormone production and fluid balance[1]. Caffeine is not a mineral but has been included in this analysis given interest in caffeine consumption from a public health perspective.
Between 2011–12 and 2023, the proportion of people with an inadequate intake:
- increased for iodine, iron and zinc
- remained similar for calcium, phosphorus and selenium
- decreased for magnesium.
More information on prevalence of inadequate mineral intakes for each sex and age group is detailed below. These results do not consider the contribution of dietary supplements to intake.
This analysis does not focus on the group average for usual mineral intakes, which is available in Table 6 from the Data downloads. Average nutrient intake based on a single day of intake is explored in more detail in the Food and nutrients release.
Calcium
Calcium is required for the growth and maintenance of bones and teeth, as well as proper functioning of the muscular and cardiovascular systems. It is required to sustain bone density and mass, meaning calcium requirements are higher for adolescents undergoing bone mass growth and for older adults experiencing bone mass deterioration (from 50 years for males and post-menopause for females). Low intakes are associated with low bone density (osteoporosis) which can increase the risk of fractured and broken bones[1]. Almost half (49.0%) of dietary calcium in 2023 came from:
- Cereal-based mixed dishes (such as sandwiches and pizza)
- Dairy milk
- Coffee and coffee substitutes
- Cheese.
Six in ten (63.7% or 15.7 million) people aged 2 years and over had an inadequate calcium intake from food and beverages in 2023. The proportion of people with an inadequate calcium intake was:
- higher for females than males (75.7% compared to 52.1%)
- lowest for children aged 2–4 years than every other age group, regardless of sex.
| Male EAR (mg/day) | Female EAR (mg/day) | Males (%) | Females (%) | |
|---|---|---|---|---|
| 2–4 | 415 | 415 | 5.3 | 10.6 |
| 5–11 | 640 | 640 | 25.3 | 38.1 |
| 12–17 | 1,050 | 1,050 | 64.8 | 93.2 |
| 18–29 | 860 | 860 | 57.3 | 81.1 |
| 30–49 | 840 | 840 | 53.2 | 70.3 |
| 50–64 | 840 | 1,085 | 48.5 | 90.7 |
| 65–74 | 945 | 1,100 | 64.7 | 87.6 |
| 75 years and over | 1,100 | 1,100 | 74.1 | 87.2 |
Proportion of people with an inadequate calcium intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","Male EAR","Female EAR","Males","Females"]
[["2\u20134","5\u201311","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[415],[640],[1050],[860],[840],[840],[945],[1100]],[[415],[640],[1050],[860],[840],[1085],[1100],[1100]],[[5.3],[25.3],[64.8],[57.3],[53.2],[48.5],[64.7],[74.1]],[[10.6],[38.1],[93.2],[81.1],[70.3],[90.7],[87.6],[87.2]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Milligrams per day (mg\/day)","axis_units":"","tooltip_units":"(mg\/day)","table_units":"(mg\/day)","axis_min":"0","axis_max":null,"tick_interval":null,"precision":"0","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]The high proportion of females aged 12–17 years and 50 years and over with an inadequate calcium intake is likely influenced by the higher calcium requirements of these age groups. Half of females aged 12–17 years had a usual calcium intake of less than 635 mg/day. This is at least 40% (415 mg/day) lower than their calcium requirements, equivalent to the amount of calcium in one and a half cups of regular fat cow’s milk.
Additionally, the low proportion of children aged 2–4 years with an inadequate calcium intake is likely the combination of lower requirements and the high popularity of Milk products and dishes (which are high in calcium[11]) for this age group.
The proportion of people with an inadequate calcium intake has remained stable over the last decade, at 61.5% in 2011–12 and 63.7% in 2023. Within age groups, the proportion of males with an inadequate calcium intake has:
- remained stable for male children aged 2–17 years (36.1% and 36.6%)
- increased for males aged 18–29 years (from 46.9% to 57.3%) and 30–49 years (from 43.2% to 53.2%)
- decreased for males aged 50–64 years (from 61.1% to 48.5%), 65–74 years (from 78.0% to 64.7%) and 75 years and over (from 88.8% to 74.1%).
| Males (%) | |
|---|---|
| 2–17(a) | 0.5 |
| 18–29 | 10.4 |
| 30–49 | 10.0 |
| 50–64 | -12.6 |
| 65–74 | -13.3 |
| 75 years and over | -14.7 |
Change in proportion of males with an inadequate calcium intake, by age, 2011–12 and 2023
["","Males"]
[["2\u201317(a)","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[0.5],[10.4],[10],[-12.6],[-13.3],[-14.7]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":"0","precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"Percentage point change (%)","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":"2","precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The apparent difference between 2011–12 and 2023 is not statistically significant.
Analysis of the distribution of calcium intakes shows that over the past decade:
- more than half of the percentiles of calcium intakes for males aged 18–29 years and 30–49 years had decreased in value, indicating a shift towards lower intakes
- more than half of the percentiles of calcium intakes for males in age groups 50 years and over had increased in value, indicating a shift towards higher intakes.
The proportion of females with an inadequate calcium intake has remained stable overall (72.7% in 2011–12 and 75.7% in 2023) but has decreased among females aged 75 years and over (from 94.1% to 87.2%).
The UL for calcium is the level at which the amount of calcium absorbed by the body may lead to hypercalcaemia, which can cause muscle weakness, excessive thirst and confusion[10]. The proportion of people with a usual calcium intake above the UL has remained steady since 2011–12 at less than 5% across all age and sex groups.
These results do not consider the contribution of dietary supplements to calcium intakes. Nutrient intakes from supplements will be included in a future Dietary supplements release.
Iodine
Iodine is a nutrient essential for producing thyroid hormones which are important for normal growth and development, particularly for the brain. Inadequate amounts of iodine may lead to a range of conditions, including goitres, hypothyroidism, and in severe cases, intellectual disability[1]. Mandatory iodine fortification (of salt used in bread and bread mixes) was implemented in Australia in 2009 to address the re-emergence of iodine deficiency[12]. Over half (53.1%) of dietary iodine in 2023 came from:
- Cereal-based mixed dishes (such as sandwiches and pizza)
- Dairy milk
- Bread and bread rolls
- Coffee and coffee substitutes.
Less than one in ten (7.4% or 1.8 million) people aged 2 years and over had an inadequate iodine intake from food and beverages in 2023. The proportion of people with an inadequate iodine intake was:
- higher for females than males in age groups between 12 and 64 years
- less than 5% for children aged between 2 and 11 years
- similar across adult male age groups (ranging between 4.4% and 6.2%)
- highest among female adults for females aged 18–29 years (17.5%), except for females aged 50–64 years (12.7%) where the difference was not significant.
| EAR (µg/day) | Males (%) | Females (%) | |
|---|---|---|---|
| 2–4(a) | 65 | 0.2 | 0.9 |
| 5–11(a) | 70 | 0.1 | 0.4 |
| 12–17 | 90 | 2.6 | 8.4 |
| 18–29 | 100 | 6.2 | 17.5 |
| 30–49 | 100 | 5.7 | 11.5 |
| 50–64 | 100 | 4.4 | 12.7 |
| 65–74 | 100 | 6.0 | 8.1 |
| 75 years and over | 100 | 4.6 | 7.4 |
Proportion of people with an inadequate iodine intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","EAR","Males","Females"]
[["2\u20134(a)","5\u201311(a)","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[65],[70],[90],[100],[100],[100],[100],[100]],[[0.2],[0.1],[2.6],[6.2],[5.7],[4.4],[6],[4.6]],[[0.9],[0.4],[8.4],[17.5],[11.5],[12.7],[8.1],[7.4]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Micrograms per day (\u00b5g\/day)","axis_units":"","tooltip_units":"(\u00b5g\/day)","table_units":"(\u00b5g\/day)","axis_min":"0","axis_max":null,"tick_interval":null,"precision":"0","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportions for ‘Males’ and ‘Females’ have high margins of error and should be used with caution.
- EAR is the same for males and females in each age group.
These results are supported by the National Health Measures Study 2022–24, which reported that the median urinary iodine concentration for adult females (101 µg/L) was lower than for adult males (123 µg/L) and for children aged 5–17 years (171 µg/L).
The high proportion of females 18–29 years who had an inadequate iodine intake may be partially due to the low proportion of this group who reported consuming Dairy milk. Almost three in ten (28.0%) females aged 18–29 years consumed Dairy milk, which was lower than any other female adult age group (ranging between 42.2% and 68.8%).
Between 2011–12 and 2023, the proportion of people with an inadequate iodine intake has increased slightly for people aged 2 years and over (from 5.1% to 7.4%). All female age groups were steady over this period, but for males there were increases among:
- males aged 18–29 years (from 1.3% to 6.2%)
- males aged 30–49 years (from 1.7% to 5.7%).
The values of only the lower percentiles of usual iodine intakes have decreased for these male age groups over this period. This change in the distribution has contributed to the increased proportion of people with an inadequate iodine intake.
In addition to inadequate iodine intakes and the resulting deficiencies, intakes above the UL can also reduce thyroid function[1]. The proportion of people who had a usual iodine intake above the UL was less than 5% in all age and sex groups.
These results do not consider the contribution of dietary supplements to iodine intakes. Nutrient intakes from supplements will be included in a future Dietary supplements release.
Iron
Iron is responsible for transporting oxygen in the blood to tissues throughout the body. It is also involved in the immune system, muscle function and cognitive functioning[13]. Iron requirements are higher for adolescents undergoing rapid growth as this, in turn, increases blood volume. In addition, iron requirements increase significantly in adult years for females due to regular blood loss during menstruation and then decrease post menopause. Inadequate iron intake may lead to iron deficiency, which can cause tiredness, poor concentration, and reduced immunity[1]. Some cereal products (such as bread and breakfast cereals) can be voluntarily fortified with iron in Australia[14]. Over one third (37.3%) of dietary iron in 2023 came from:
- Cereal-based mixed dishes (such as sandwiches and pasta/noodle dishes)
- Ready to eat breakfast cereals
- Bread and bread rolls.
Almost two in ten (17.3% or 4.3 million) people aged 2 years and over had an inadequate iron intake from food and beverages in 2023. The proportion of people with an inadequate iron intake was:
- three times higher for females than males (26.8% compared to 8.2%)
- similar for all male age groups (between 7.0% and 10.9%)
- higher for females aged 12–17 years (37.2%), 18–29 years (47.7%) and 30–49 years (42.2%) than females in all other age groups.
| Male EAR (mg/day) | Female EAR (mg/day) | Males (%) | Females (%) | |
|---|---|---|---|---|
| 2–4 | 4 | 4 | 10.9 | 16.4 |
| 5–11 | 5 | 5 | 8.0 | 12.8 |
| 12–17 | 7 | 7 | 9.5 | 37.2 |
| 18–29 | 6 | 8 | 8.1 | 47.7 |
| 30–49 | 6 | 8 | 8.0 | 42.2 |
| 50–64 | 6 | 5 | 7.9 | 9.8 |
| 65–74 | 6 | 5 | 7.9 | 9.9 |
| 75 years and over | 6 | 5 | 7.0 | 9.4 |
Proportion of people with an inadequate iron intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","Male EAR","Female EAR","Males","Females"]
[["2\u20134","5\u201311","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[4],[5],[7],[6],[6],[6],[6],[6]],[[4],[5],[7],[8],[8],[5],[5],[5]],[[10.9],[8],[9.5],[8.1],[8],[7.9],[7.9],[7]],[[16.4],[12.8],[37.2],[47.7],[42.2],[9.8],[9.9],[9.4]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Milligrams per day (mg\/day)","axis_units":"","tooltip_units":"(mg\/day)","table_units":"(mg\/day)","axis_min":"0","axis_max":null,"tick_interval":"1","precision":"0","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]These results are supported by the National Health Measures Study 2022–24, which reported that the mean serum ferritin level was higher for males than females in every age group, and that female adults were more likely to be ferritin deficient than male adults (5.6% compared to 0.9%).
Almost one in two (47.7%) females aged 18–29 years did not meet their iron requirements in 2023. This high proportion reflects the combination of:
- high iron requirements (8 mg/day)
- a lower average usual iron intake (8 mg/day) for this age group compared to other female adult age groups (9 mg/day).
Similarly, over one in three females aged 12–17 years (37.2%) and 30–49 years (42.2%) did not meet their iron requirements. These age groups have:
- higher iron requirements (7 mg/day and 8 mg/day) than females aged 50 years and over (5 mg/day)
- a similar average usual iron intake (9 mg/day) to females aged 50 years and over (also 9 mg/day).
The high proportion of females aged 12–17 years and 30–49 years with an inadequate iron intake when compared to females aged 50 years and over likely reflects the higher iron requirements rather than differences in intake.
The proportion of children aged 12–17 years who had an inadequate iron intake was over three times higher for females than males (37.2% compared to 9.5%), even though they have the same requirements. This may be partly due to the higher proportion of males in this age group who reported consuming Ready to eat breakfast cereals, many of which are high iron (34.9% compared to 22.8%). Additionally, of people aged 12–17 years who consumed Ready to eat breakfast cereals, males consumed a larger median amount than females (69 g compared to 51 g).
The proportion of people with an inadequate iron intake has increased over the last decade from 13.2% in 2011–12 to 17.3% in 2023, reflecting the increase in the proportion of adults with an inadequate iron intake.
The proportion of males with an inadequate iron intake has:
- remained steady for children aged 2–17 years and older males aged 75 years and over
- increased for all male age groups between 18 and 74 years.
These changes over time have meant that the proportion of males with an inadequate iron intake is now similar across all male age groups, whereas in 2011–12, male children were more likely to have an inadequate iron intake than male adults.
| Males 2011–12 (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | Males 2023 (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | |
|---|---|---|---|---|---|---|
| 2–4 | 8.4 | 6.3 | 10.5 | 10.9 | 8.1 | 13.7 |
| 5–11 | 6.5 | 4.3 | 8.7 | 8.0 | 5.0 | 11.0 |
| 12–17 | 7.2 | 4.1 | 10.3 | 9.5 | 6.5 | 12.5 |
| 18–29 | 2.2 | 1.7 | 2.7 | 8.1 | 5.4 | 10.8 |
| 30–49 | 2.4 | 1.1 | 3.7 | 8.0 | 5.7 | 10.3 |
| 50–64 | 2.9 | 2.7 | 3.1 | 7.9 | 5.7 | 10.1 |
| 65–74 | 2.6 | 0.5 | 4.7 | 7.9 | 5.2 | 10.6 |
| 75 years and over | 3.8 | 2.2 | 5.4 | 7.0 | 3.5 | 10.5 |
Proportion of males with an inadequate iron intake, by age, 2011–12 and 2023
["","Males 2011\u201312","95% confidence interval","Males 2023","95% confidence interval"]
[["2\u20134","5\u201311","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[8.4],[6.5],[7.2],[2.2],[2.4],[2.9],[2.6],[3.8]],[[6.3,10.5],[4.3,8.7],[4.1,10.3],[1.7,2.7],[1.1,3.7],[2.7,3.1],[0.5,4.7],[2.2,5.4]],[[10.9],[8],[9.5],[8.1],[8],[7.9],[7.9],[7]],[[8.1,13.7],[5,11],[6.5,12.5],[5.4,10.8],[5.7,10.3],[5.7,10.1],[5.2,10.6],[3.5,10.5]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]Analysis of the distribution of iron intakes shows that all male adult age groups had lower intakes across more than half of their percentiles of usual iron intakes over the past decade, indicating a shift towards lower intakes.
Over the past decade, the proportion of females with an inadequate iron intake has:
- remained steady for females aged 2–17 years, 30–49 years and 75 years and over
- increased for females aged 18–29 years, 50–64 years and 65–74 years.
The increase in the proportion of females aged 18–29 years, 50–64 years and 65–74 years with an inadequate iron intake reflects a decrease of about 1-2 mg/day across most percentiles of usual iron intakes in these age groups.
| Females 2011–12 (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | Females 2023 (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | |
|---|---|---|---|---|---|---|
| 2–4 | 14.4 | 11.8 | 17.0 | 16.4 | 12.2 | 20.6 |
| 5–11 | 11.4 | 9.3 | 13.5 | 12.8 | 9.1 | 16.5 |
| 12–17 | 34.9 | 29.7 | 40.1 | 37.2 | 31.8 | 42.6 |
| 18–29 | 38.1 | 33.6 | 42.6 | 47.7 | 43.6 | 51.8 |
| 30–49 | 37.5 | 34.3 | 40.7 | 42.2 | 38.7 | 45.7 |
| 50–64 | 5.4 | 3.5 | 7.3 | 9.8 | 7.8 | 11.8 |
| 65–74 | 5.8 | 4.6 | 7.0 | 9.9 | 7.8 | 12.0 |
| 75 years and over | 6.5 | 4.5 | 8.5 | 9.4 | 6.2 | 12.6 |
Proportion of females with an inadequate iron intake, by age, 2011–12 and 2023
["","Females 2011\u201312","95% confidence interval","Females 2023","95% confidence interval"]
[["2\u20134","5\u201311","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[14.4],[11.4],[34.9],[38.1],[37.5],[5.4],[5.8],[6.5]],[[11.8,17],[9.3,13.5],[29.7,40.1],[33.6,42.6],[34.3,40.7],[3.5,7.3],[4.6,7],[4.5,8.5]],[[16.4],[12.8],[37.2],[47.7],[42.2],[9.8],[9.9],[9.4]],[[12.2,20.6],[9.1,16.5],[31.8,42.6],[43.6,51.8],[38.7,45.7],[7.8,11.8],[7.8,12],[6.2,12.6]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]As the body has no way to remove excess iron consumed in the diet, intakes above the UL can cause iron to build up in the internal organs and joints, eventually leading to organ damage[15]. In 2023, the proportion of people who had a usual iron intake above the UL was less than 5% in all age and sex groups.
These results do not consider the contribution of dietary supplements to iron intakes. Nutrient intake from supplements will be included in a future Dietary supplements release.
Magnesium
Magnesium is required for a range of activities in the human body including protein production, muscle and nerve function, blood glucose control and bone development. From adolescence, magnesium requirements are higher for males than females in each age group due to increased metabolic demands. The effects of deficiency are rare but can include muscular weakness and spasms, lethargy, and hyper-irritability[1]. The leading sources of dietary magnesium in 2023 were:
- Cereal-based mixed dishes (such as sandwiches and pasta/noodle dishes) (12.9%)
- Water (9.5%)
- Coffee and coffee substitutes for adults (7.7%) and Ready to eat breakfast cereals for children (5.7%).
Three in ten (31.3% or 7.7 million) people aged 2 years and over had an inadequate magnesium intake from food and beverages in 2023. The proportion of people with an inadequate magnesium intake was:
- higher for males than females (35.2% compared to 27.3%)
- higher for adults than children (35.9% compared to 13.5%)
- less than 5.0% for children aged between 2 and 11 years.
| Male EAR (mg/day) | Female EAR (mg/day) | Males (%) | Females (%) | |
|---|---|---|---|---|
| 2–4(a) | 80 | 80 | 0.0 | 0.0 |
| 5–11(a) | 150 | 150 | 0.4 | 1.4 |
| 12–17 | 295 | 265 | 26.8 | 43.9 |
| 18–29 | 330 | 260 | 40.8 | 37.3 |
| 30–49 | 350 | 265 | 41.4 | 26.0 |
| 50–64 | 350 | 265 | 38.6 | 26.4 |
| 65–74 | 350 | 265 | 45.6 | 28.1 |
| 75 years and over | 350 | 265 | 50.2 | 39.6 |
Proportion of people with an inadequate magnesium intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","Male EAR","Female EAR","Males","Females"]
[["2\u20134(a)","5\u201311(a)","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[80],[150],[295],[330],[350],[350],[350],[350]],[[80],[150],[265],[260],[265],[265],[265],[265]],[[0],[0.4],[26.8],[40.8],[41.4],[38.6],[45.6],[50.2]],[[0],[1.4],[43.9],[37.3],[26],[26.4],[28.1],[39.6]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Milligrams per day (mg\/day)","axis_units":"","tooltip_units":"(mg\/day)","table_units":"(mg\/day)","axis_min":"0","axis_max":null,"tick_interval":null,"precision":"0","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportions for ‘Males’ and ‘Females’ have high margins of error and should be used with caution.
Although magnesium requirements are similar across female age groups from 12 years and over, the proportion of females with an inadequate magnesium intake was lower among females aged between 30 and 74 years (between 26.0% and 28.1%). This is reflected in the median and most other percentiles of usual magnesium intakes, which are between 20 and 48 mg/day higher for females in these groups than for females aged 12–17 years, 18–29 years, and 75 years and over.
| 12–17 years (mg/day) | 18–29 years (mg/day) | 30–49 years (mg/day) | 50–64 years (mg/day) | 65–74 years (mg/day) | 75 years and over (mg/day) | |
|---|---|---|---|---|---|---|
| 25th percentile | 229 | 235 | 263 | 262 | 259 | 236 |
| 50th percentile (median) | 276 | 283 | 314 | 313 | 309 | 284 |
| 75th percentile | 330 | 336 | 371 | 369 | 365 | 337 |
Percentiles of usual magnesium intake for females, by age, 2023
["","12\u201317 years","18\u201329 years","30\u201349 years","50\u201364 years","65\u201374 years","75 years and over"]
[["25th percentile","50th percentile (median)","75th percentile"],[[229],[276],[330]],[[235],[283],[336]],[[263],[314],[371]],[[262],[313],[369]],[[259],[309],[365]],[[236],[284],[337]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Percentile","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"Milligrams per day (mg\/day)","axis_units":"","tooltip_units":"(mg\/day)","table_units":"(mg\/day)","axis_min":null,"axis_max":null,"tick_interval":"50","precision":"0","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]The proportion of people with an inadequate magnesium intake has decreased slightly from 34.9% in 2011–12 to 31.3% in 2023. Within age groups, the proportions have remained mostly similar, although there were decreases among:
- children aged 12–17 years (from 44.5% to 26.8% for males, and from 57.3% to 43.9% for females)
- males aged 75 years and over (from 65.7% to 50.2%)
- females aged 30–49 years (from 33.8% to 26.0%)
- females aged 65–74 years (from 39.3% to 28.1%).
The decrease in the proportion of people with an inadequate magnesium intake is reflective of the increase in the value of the:
- lower percentiles for females aged 12–17 years, 30–49 years and 65–74 years
- upper percentiles for males aged 5–11 years, 12–17 years, 50–64 years and 75 years and over.
These results do not consider the contribution of dietary supplements to magnesium intakes. Nutrient intake from supplements will be included in a future Dietary supplements release.
Phosphorous
Phosphorus plays an important role in the formation of bones and teeth, protein production and energy-producing activities in cells. Deficiencies can lead to muscle weakness, rickets, ataxia, and confusion. Phosphorus requirements for adolescents are significantly higher than for adults because of the additional phosphorus required during periods of rapid growth[1]. One-third (34.6%) of dietary phosphorus in 2023 came from:
- Cereal-based mixed dishes (such as sandwiches, pizza and burgers)
- Dairy milk
- Coffee and coffee substitutes
- Poultry-based mixed dishes.
Almost all (98.0%) people aged 2 years and over had usual phosphorus intake from food and beverages that met their requirements. The proportion of people with an inadequate phosphorus intake was:
- less than 5% across almost all sex and age groups
- 7.3% for males aged 12–17 years and 33.9% for females aged 12–17 years.
As children aged 12–17 years had a similar average usual intake of phosphorus as most of the adult age groups, the high proportion of 12–17 year olds with an inadequate phosphorus intake is likely due to the greater requirements of this age group rather than differences in intake.
| EAR(c) (mg/day) | Males (%) | Females (%) | |
|---|---|---|---|
| 2–4(a) | 390 | 0.0 | 0.1 |
| 5–11(b) | 685 | 0.6 | 2.5 |
| 12–17 | 1,055 | 7.3 | 33.9 |
| 18–29(b) | 620 | 0.3 | 1.4 |
| 30–49(a) | 580 | 0.2 | 0.4 |
| 50–64(a) | 580 | 0.2 | 0.5 |
| 65–74(a) | 580 | 0.3 | 0.4 |
| 75 years and over(a) | 580 | 0.3 | 0.7 |
Proportion of people with an inadequate phosphorus intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","EAR(c)","Males","Females"]
[["2\u20134(a)","5\u201311(b)","12\u201317","18\u201329(b)","30\u201349(a)","50\u201364(a)","65\u201374(a)","75 years and over(a)"],[[390],[685],[1055],[620],[580],[580],[580],[580]],[[0],[0.6],[7.3],[0.3],[0.2],[0.2],[0.3],[0.3]],[[0.1],[2.5],[33.9],[1.4],[0.4],[0.5],[0.4],[0.7]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Milligrams per day (mg\/day)","axis_units":"","tooltip_units":"(mg\/day)","table_units":"(mg\/day)","axis_min":"0","axis_max":null,"tick_interval":null,"precision":"0","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportions for ‘Males’ and ‘Females’ have high margins of error and should be used with caution.
- The proportion for ‘Males’ has a high margin of error and should be used with caution.
- EAR is the same for males and females in each age group.
The proportion of people who had an inadequate phosphorus intake has remained stable since the last decade for each age group.
Among people who have chronic kidney disease (CKD) or cardiovascular disease (CVD), high phosphorus intakes can lead to hyperphosphataemia, which is often asymptomatic but can cause muscle spasms, nausea and chronic kidney failure[16]. In 2023, the proportion of people who had a usual phosphorus intake above the UL was less than 5% for all age and sex groups.
These results do not consider the contribution of dietary supplements to phosphorus intakes. Nutrient intakes from supplements will be included in a future Dietary supplements release.
Selenium
Selenium functions as an antioxidant and is important in thyroid metabolism. Selenium levels can vary widely depending on soil concentrations. Requirements are linked to body weight and metabolism and, as a result, are lower for young children but similar between adolescents and adults. Requirements are also slightly higher for adult males than adult females. Deficiencies are rare in Australia but can lead to Keshan disease, which causes enlargement of the heart, heart failure, arrythmias, and premature death[1]. Over one-third (38.0%) of dietary selenium in 2023 came from:
- Cereal-based mixed dishes (like sandwiches, pasta/noodle dishes, pizza and burgers)
- Poultry and feathered game
- Poultry-based mixed dishes
- Water.
One in twenty (5.3% or 1.3 million) people aged 2 years and over had an inadequate selenium intake in 2023. The proportion of people with an inadequate selenium intake was:
- less than 5% of children aged 2–17 years, regardless of sex
- generally similar across age groups for adult males between 18 and 74 years (between 4.6% and 9.3%)
- similar across most female age groups from 18 years onwards (between 4.5% and 11.7%).
| Male EAR (µg/day) | Female EAR (µg/day) | Males (%) | Females (%) | |
|---|---|---|---|---|
| 2–4(a) | 20 | 20 | 0.0 | 0.0 |
| 5–11(a) | 30 | 30 | 0.0 | 0.1 |
| 12–17 | 55 | 45 | 2.7 | 4.1 |
| 18–29 | 60 | 50 | 5.0 | 8.3 |
| 30–49 | 60 | 50 | 4.6 | 4.5 |
| 50–64 | 60 | 50 | 5.4 | 5.8 |
| 65–74 | 60 | 50 | 9.3 | 6.8 |
| 75 years and over | 60 | 50 | 12.9 | 11.7 |
Proportion of people with an inadequate selenium intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","Male EAR","Female EAR","Males","Females"]
[["2\u20134(a)","5\u201311(a)","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[20],[30],[55],[60],[60],[60],[60],[60]],[[20],[30],[45],[50],[50],[50],[50],[50]],[[0],[0],[2.7],[5],[4.6],[5.4],[9.3],[12.9]],[[0],[0.1],[4.1],[8.3],[4.5],[5.8],[6.8],[11.7]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Micrograms per day (\u00b5g\/day)","axis_units":"","tooltip_units":"(\u00b5g\/day)","table_units":"(\u00b5g\/day)","axis_min":"0","axis_max":null,"tick_interval":null,"precision":"0","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportions for ‘Males’ and ‘Females’ have high margins of error and should be used with caution.
Between 2011–12 and 2023, the proportion of people with an inadequate selenium intake has remained similar for all sex and age groups.
Selenium intakes above the UL can lead to brittle hair and nails, gastrointestinal disturbance and nervous system abnormalities[1]. The proportion of people with a usual selenium intake above the UL was less than 5% for all age and sex groups in 2023.
These results do not consider the contribution of dietary supplements to selenium intakes. Nutrient intakes from supplements will be included in a future Dietary supplements release.
Sodium
Sodium helps regulate body fluids, nerve health and electrolyte balance. Sodium intake is closely related to blood pressure and high intakes can cause hypertension (high blood pressure), which is a risk factor for developing heart and kidney disease[1]. Sodium is found in different forms in our food but is generally consumed as sodium chloride (salt). Over one third (42.1%) of dietary sodium in 2023 came from:
- Cereal-based mixed dishes (such as sandwiches and pizza)
- Bread and bread rolls
- Processed meat
- Poultry-based mixed dishes.
Nearly two in three (65.6% or 12.9 million) adults aged 18 years and over had a usual sodium intake from food and beverages above the Suggested Dietary Target (SDT) of 2,000 mg/day in 2023. Across age and sex, the proportion was:
- higher for males than females (79.9% compared to 51.2%), including within every age group
- highest among males aged 18–29 years (88.2%) compared to any other male age group, except for males aged 30–49 years (81.5%) where the difference was not significant
- higher for females aged 18–29 years and 30–49 years (59.6% and 56.8%) than for females aged 65–74 years and 75 years and over (44.2% and 35.4%).
| Males (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | Females (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | |
|---|---|---|---|---|---|---|
| 18–29 | 88.2 | 82.6 | 93.8 | 59.6 | 50.4 | 68.8 |
| 30–49 | 81.5 | 77.0 | 86.0 | 56.8 | 51.8 | 61.8 |
| 50–64 | 78.5 | 72.7 | 84.3 | 47.4 | 39.2 | 55.6 |
| 65–74 | 71.2 | 64.5 | 77.9 | 44.2 | 37.7 | 50.7 |
| 75 years and over | 68.1 | 60.5 | 75.7 | 35.4 | 28.3 | 42.5 |
Proportion of adults with a usual sodium intake above the Suggested Dietary Target (SDT)(a), by age and sex, 2023
["","Males","95% confidence interval","Females","95% confidence interval"]
[["18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[88.2],[81.5],[78.5],[71.2],[68.1]],[[82.6,93.8],[77,86],[72.7,84.3],[64.5,77.9],[60.5,75.7]],[[59.6],[56.8],[47.4],[44.2],[35.4]],[[50.4,68.8],[51.8,61.8],[39.2,55.6],[37.7,50.7],[28.3,42.5]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- SDT is 2,000mg/day for adults aged 18 years and over.
The average usual intake of sodium for males aged 18–29 years (3,021 mg/day) was:
- higher than any other adult male age group (between 2,420 mg/day and 2,771 mg/day)
- 50% higher than the SDT.
Since 2011–12, the proportion of adults who had a usual sodium intake above the SDT has decreased for males (from 84.8% to 79.9%) but remained similar for females (54.2% and 51.2%).
As the SDT only applies to adults, it is useful to consider usual sodium intakes for children. The average usual sodium intake for children was:
- among males, higher for males aged 12–17 years (3,247 mg/day) than for 2–4 years and 5–11 years (1,604 mg/day and 2,290 mg/day)
- among females, higher for females aged 12–17 years (2,405 mg/day) than 2–4 years and 5–11 years (1,437 mg/day and 2,072 mg/day).
This analysis may underestimate total sodium intakes, as it only accounts for sodium naturally present in foods or added during processing. Based on responses about additional salt use, 78.1% people aged 2 years and over added salt while cooking or preparing food and 45.5% added salt to food at the table.
Zinc
Zinc is involved in a variety of body processes, ranging from helping maintain the structural integrity of proteins to regulating gene expression. Zinc requirements account for the relationship between zinc absorption and loss (which differs by age and sex) and are almost twice as high for males than females in adolescence and adulthood. Deficiencies can cause delayed growth, impaired immune responses, alopecia and eye and skin lesions[1]. Over one third (41.0%) of dietary zinc in 2023 came from:
- Cereal-based mixed dishes (such as sandwiches and pasta/noodle dishes)
- Beef, sheep and pork, unprocessed
- Beef, sheep and pork-based mixed dishes
- Ready to eat breakfast cereals.
Three in ten (29.7% or 7.3 million) people aged 2 years and over had an inadequate zinc intake in 2023. The proportion of people with an inadequate zinc intake was:
- less than 5% for children aged 2–4 and 5–11 years
- more than four times higher for males than females (47.7% compared to 11.2%)
- higher for males than females in every age group above 12 years, particularly among adult age groups.
| Male EAR (mg/day) | Female EAR (mg/day) | Males (%) | Females (%) | |
|---|---|---|---|---|
| 2–4(a) | 2.7 | 2.7 | 0.0 | 0.1 |
| 5–11(a) | 3.9 | 3.9 | 0.1 | 0.4 |
| 12–17 | 9.0 | 5.7 | 16.8 | 7.2 |
| 18–29 | 11.9 | 6.5 | 55.3 | 15.8 |
| 30–49 | 12.0 | 6.5 | 54.9 | 10.9 |
| 50–64 | 12.0 | 6.5 | 60.1 | 12.9 |
| 65–74 | 12.0 | 6.5 | 65.4 | 13.1 |
| 75 years and over | 12.0 | 6.5 | 68.9 | 18.6 |
Proportion of people with an inadequate zinc intake and weighted Estimated Average Requirement (EAR), by age and sex, 2023
["","Male EAR","Female EAR","Males","Females"]
[["2\u20134(a)","5\u201311(a)","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[2.7],[3.9],[9],[11.9],[12],[12],[12],[12]],[[2.7],[3.9],[5.7],[6.5],[6.5],[6.5],[6.5],[6.5]],[[0],[0.1],[16.8],[55.3],[54.9],[60.1],[65.4],[68.9]],[[0.1],[0.4],[7.2],[15.8],[10.9],[12.9],[13.1],[18.6]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false},{"value":"1","axis_id":"1","axis_title":"Milligrams per day (mg\/day)","axis_units":"","tooltip_units":"(mg\/day)","table_units":"(mg\/day)","axis_min":"0","axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportions for ‘Males’ and ‘Females’ have high margins of error and should be used with caution.
Among adults, 25% of males had a usual zinc intake of less than 9.5 mg/day (25th percentile). This is at least 20% below (or around 2.5 mg/day) the zinc requirements for adult male age groups 30 years and over (12.0 mg/day).
The proportion of people with an inadequate zinc intake has increased from 22.7% in 2011–12 to 29.7% in 2023. When comparing across age, the pattern of people with an inadequate zinc intake has varied between males and females over the last 10 years.
Between 2011–12 and 2023, the proportion of males with an inadequate zinc intake has:
- remained similar for children aged 2–4 years (less than 5%), 5–11 years (less than 5%), and 12–17 years (11.2% and 16.8%)
- increased for all age groups between 18 and 74 years
- remained similar for males aged 75 years and over (69.3% and 68.9%).
| Males 2011–12 (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | Males 2023 (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | |
|---|---|---|---|---|---|---|
| 2–4(a) | 0.0 | 0.0 | ||||
| 5–11(a) | 0.0 | 0.1 | ||||
| 12–17 | 11.2 | 5.0 | 17.4 | 16.8 | 11.1 | 22.5 |
| 18–29 | 35.9 | 28.6 | 43.2 | 55.3 | 47.7 | 62.9 |
| 30–49 | 40.0 | 33.5 | 46.5 | 54.9 | 49.3 | 60.5 |
| 50–64 | 49.9 | 43.7 | 56.1 | 60.1 | 53.5 | 66.7 |
| 65–74 | 53.5 | 45.5 | 61.5 | 65.4 | 59.2 | 71.6 |
| 75 years and over | 69.3 | 60.8 | 77.8 | 68.9 | 61.3 | 76.5 |
Proportion of males with an inadequate zinc intake, by age, 2011–12 and 2023
["","Males 2011\u201312","95% confidence interval","Males 2023","95% confidence interval"]
[["2\u20134(a)","5\u201311(a)","12\u201317","18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[0],[0],[11.2],[35.9],[40],[49.9],[53.5],[69.3]],[[null],[null],[5,17.4],[28.6,43.2],[33.5,46.5],[43.7,56.1],[45.5,61.5],[60.8,77.8]],[[0],[0.1],[16.8],[55.3],[54.9],[60.1],[65.4],[68.9]],[[null],[null],[11.1,22.5],[47.7,62.9],[49.3,60.5],[53.5,66.7],[59.2,71.6],[61.3,76.5]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]- The proportions for ‘Males 2011–12’ and ‘Males 2023’ have high margins of error and should be used with caution.
Analysis of the distribution of zinc intakes shows that males in age groups between 18 and 74 years had lower intakes across most of the percentiles of usual zinc intake in 2023 than in 2011–12, which has contributed to the increased proportion of males with inadequate zinc intakes in these groups.
The proportion of females with an inadequate zinc intake between 2011–12 and 2023 has remained stable overall (9.0% and 11.2%) but has increased among females aged 75 years and over (from 10.8% to 18.6%).
In addition to inadequate intakes, long term zinc intakes above the UL can lead to decreased immunity and copper deficiency[1]. In 2023, one in ten (10.9%) male children aged 2–4 years had a usual zinc intake above the UL. The proportion for all other age and sex groups was less than 5%.
These results do not consider the contribution of dietary supplements to zinc intakes. Nutrient intake from supplements will be included in a future Dietary supplements publication.
Caffeine
Caffeine is a stimulant that is both found naturally and commonly added to some foods and beverages[17]. Common side effects of consuming too much caffeine include an increased heart rate, anxiety and sleep disturbances[18]. Most (92.6%) dietary caffeine in 2023 came from:
- Coffee and coffee substitutes
- Tea
- Soft drinks and flavoured mineral waters.
The average usual caffeine intake has increased for most adult age groups between 2011–12 and 2023. Across age groups, intakes were lower among children than adults and increased with each age group from 18 years onwards until 50 years for males and 30 years for females.
There are no NRVs for caffeine, however it is generally recommended that:
- children aged 2–11 years limit their caffeine intake to 3 mg/kg of body weight
- people aged 12 years and over limit their caffeine intake to 5.7 mg/kg of body weight[19].
When adjusted for body weight, the proportion of males who had a usual caffeine intake above the suggested safe level of intake was:
- less than 5% for males aged under 50 years
- similar across male age groups from 50 years and over (ranging from 5.0% to 5.6%).
Similarly, the proportion of females who had a usual caffeine intake above the suggested safe level of intake was:
- less than 5% for females aged under 30 years
- similar across female age groups from 30 years and over (ranging from 6.3% to 8.4%).
| Males (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | Females (%) | 95% confidence interval (%) (low) | 95% confidence interval (%) (high) | |
|---|---|---|---|---|---|---|
| 18–29 | 1.2 | 0.2 | 2.2 | 1.7 | 0.4 | 3.0 |
| 30–49 | 3.3 | 1.9 | 4.7 | 6.3 | 4.1 | 8.5 |
| 50–64 | 5.0 | 2.9 | 7.1 | 7.1 | 4.6 | 9.6 |
| 65–74 | 5.6 | 3.3 | 7.9 | 8.4 | 5.9 | 10.9 |
| 75 years and over | 5.6 | 2.4 | 8.8 | 8.0 | 5.4 | 10.6 |
Proportion of adults with a usual caffeine intake above the suggested safe level of intake, by age and sex, 2023
["","Males","95% confidence interval","Females","95% confidence interval"]
[["18\u201329","30\u201349","50\u201364","65\u201374","75 years and over"],[[1.2],[3.3],[5],[5.6],[5.6]],[[0.2,2.2],[1.9,4.7],[2.9,7.1],[3.3,7.9],[2.4,8.8]],[[1.7],[6.3],[7.1],[8.4],[8]],[[0.4,3],[4.1,8.5],[4.6,9.6],[5.9,10.9],[5.4,10.6]]]
[]
[{"value":"0","axis_id":"0","axis_title":"Age group (years)","axis_units":"","tooltip_units":"","table_units":"","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"-1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}][{"value":"0","axis_id":"0","axis_title":"%","axis_units":"","tooltip_units":"(%)","table_units":"(%)","axis_min":null,"axis_max":null,"tick_interval":null,"precision":"1","data_unit_prefix":"","data_unit_suffix":"","reverse_axis":false}]Footnotes
- Eat for Health, ‘Nutrient Reference Values for Australia and New Zealand', https://www.nhmrc.gov.au/about-us/publications/nutrient-reference-values-australia-and-new-zealand-including-recommended-dietary-intakes; accessed 06/02/2026.
- Food Standards Australia New Zealand (FSANZ), ‘Principles and Practices of Dietary Exposure Assessment for Food Regulatory Purposes', https://www.foodstandards.gov.au/publications/principles-and-practices-of-dietary-exposure-assessment; accessed 06/02/2026.
- World Health Organization, ‘Guideline: Sugars intake for adults and children', https://www.who.int/publications/i/item/9789241549028; accessed 06/02/2026.
- Eat for Health, ‘Discretionary food and drink choices', https://www.eatforhealth.gov.au/food-essentials/discretionary-food-and-drink-choices; accessed 06/02/2026.
- Dietitians Australia, ‘Protein’, https://dietitiansaustralia.org.au/health-advice/protein; accessed 06/02/2026.
- World Health Organization, ‘Micronutrients’, https://www.who.int/health-topics/micronutrients; accessed 06/02/2026.
- Food Standards Australia and New Zealand, ‘Thiamin fortification', https://www.foodstandards.gov.au/consumer/food-fortification/thiamin-fortification; accessed 06/02/2026.
- Therapeutic Goods Administration, 'Vitamin B6 (pyridoxine)', https://www.tga.gov.au/news/safety-alerts/vitamin-b6-pyridoxine; accessed 06/02/2026.
- Food Standards Australia New Zealand, ‘Folic acid fortification', https://www.foodstandards.gov.au/consumer/food-fortification/folic-acid/mandatory; accessed 06/02/2026.
- Cancer Australia, ‘Hypercalcaemia', https://www.canceraustralia.gov.au/cancer-types/breast-cancer/living-breast-cancer/managing-physical-changes-women-metastatic-breast-6; accessed 06/02/2026.
- Eat for Health, ‘Milk, yoghurt, cheese and/or their alternatives (mostly reduced fat)’, https://www.eatforhealth.gov.au/food-essentials/five-food-groups/milk-yoghurt-cheese-andor-their-alternatives-mostly-reduced-fat; accessed 06/02/2026.
- Food Standards Australia New Zealand, ‘Iodine fortification', https://www.foodstandards.gov.au/consumer/food-fortification/iodine-fortification; accessed 06/02/2026.
- Dietitians Australia, ‘Dietary iron makes health bodies', https://dietitiansaustralia.org.au/health-advice/dietary-iron-makes-healthy-bodies; accessed 06/02/2026.
- Food Standards Australia and New Zealand, ‘Vitamins and minerals added to food', https://www.foodstandards.gov.au/consumer/food-fortification/vitamin-added; accessed 06/02/2026.
- Haemochromatosis Australia, ‘Haemochromatosis', https://haemochromatosis.org.au/haemochromatosis/; accessed 06/02/2026.
- The Royal Children’s Hospital Melbourne, ‘Hyperphosphataemia', https://www.rch.org.au/clinicalguide/guideline_index/Hyperphosphataemia/; accessed 06/02/2026.
- Food Standards Australia New Zealand, ‘Caffeine', https://www.foodstandards.gov.au/consumer/prevention-of-foodborne-illness/caffeine; accessed 06/02/2026.
- NSW Health, ‘Energy drinks and caffeine', https://www.health.nsw.gov.au/aod/resources/Pages/energy-drinks.aspx; accessed 06/02/2026.
- Food Standards Australia New Zealand, ‘Supporting document 1 – Safety assessment of caffeine', https://www.foodstandards.gov.au/sites/default/files/food-standards-code/proposals/Documents/P1056%20SD1%201st%20CFS%20Safety%20Assessment.pdf; accessed 06/02/2026.
Data downloads
See National Nutrition and Physical Activity 2023 data downloads for the full suite of available data.
Data relating to usual nutrient intakes can be found in tables:
- TABLES 1–3 Summary of usual nutrient intake compared to Nutrient Reference Values (NRVs), by age and sex
- TABLE 4 Usual intake of macronutrients and moisture, by age and sex
- TABLE 5 Usual intake of vitamins, by age and sex
- TABLE 6 Usual intake of minerals, by age and sex
- TABLE 7 Usual proportion of energy from macronutrients, by age and sex.
Methodology
Scope
Includes:
- usual residents in Australia aged 2+ years living in private dwellings
- urban and rural areas in all states and territories, excluding very remote parts of Australia and discrete Aboriginal and Torres Strait Islander Communities.
Geography
The data available includes estimates for Australia.
Source
The National Nutrition and Physical Activity Survey conducted by the Australian Bureau of Statistics.
Collection method
- Face-to-face interview with an ABS Interviewer
- 24-hour dietary recall data collected face-to-face with an ABS Interviewer or via an online interview
- Some physical activity and sleep data was collected on a voluntary basis via an accelerometer.
Concepts, sources and methods
- Descriptions of the concepts underlying the data are available in IHMHS: Concepts, Sources and Methods
- 24-hour dietary recall is presented using a classification based on the AUSNUT files by FSANZ.