|
|
INTRODUCTION
This publication provides a brief overview of the prevalence, risk factors, disability and other factors for persons with musculoskeletal disorders in Australia. The publication draws on data from the 2004-05 National Health Survey (NHS), ABS Causes of Death collection, the 2003 ABS Survey of Disability, Ageing and Carers, the 2004-05 National Aboriginal and Torres Strait Islander Health Survey and other ABS and non-ABS sources.
DATA SOURCES
Unless otherwise stated this article presents information sourced from the 2004-05 NHS. Respondents were asked if they had ever been diagnosed with arthritis or osteoporosis by a doctor or a nurse.
In this publication, where data are referenced from the ABS 2004-05 NHS, arthritis refers to osteoarthritis, rheumatoid arthritis and other forms of arthritis including type unknown. Back problems refers to back pain and problems and disc disorders that have lasted, or are expected to last, for six months or more. A person may have reported having more than one of these musculoskeletal conditions as a long-term condition. A long term condition is a current condition which has lasted or was expected to last for six months or more.
As for any self-reported condition, the quality of responses to surveys depends on the consistency with which respondents can report a particular condition. Conditions such as arthritis and rheumatism are relatively common terms which are used to refer to pain associated with the joints. Changing public awareness and acceptance of the condition, and associated services, may also affect respondents' tendency to report it.
INQUIRIES
For further information about these and related statistics, contact the National Information and Referral Service on 1300 135 070 or email client.services@abs.gov.au.
MUSCULOSKELETAL CONDITIONS
Musculoskeletal conditions are defined as conditions of the bones, muscles and their attachments, and include joint problems such as arthritis. Although there are more than one hundred musculoskeletal conditions the most common are osteoarthritis, rheumatoid arthritis, osteoporosis and back pain (AIHW 2004).
In 2004-05, musculoskeletal conditions, as reported in the NHS, were more prevalent than any other of the National Health Priority Areas (NHPAs), with 31% of Australians suffering from one or more of these conditions. Arthritis and musculoskeletal conditions were also responsible for the main disabling condition in more than one in three Australians with a disability (ABS 2004), and were a major area of health expenditure in 2001-02, with around $4.6 billion spent on the conditions (AIHW 2004).
COMMON MUSCULOSKELETAL CONDITIONS
- Arthritis is characterised by inflammation of the joints, often resulting in pain, stiffness, disability and deformity. The two most common types of arthritis are osteoarthritis and rheumatoid arthritis.
- Osteoarthritis is a degenerative joint condition affecting the weight-bearing joints such as the hips, knees and ankles as well as the hands and spine. In the initial stages pain occurs in the joints during and after activity but as the condition progresses pain may be experienced from minimal movement or during rest (AIHW 2005).
- Rheumatoid arthritis is an auto-immune disease causing chronic inflammation of the joints. It most commonly affects the hand joints and can lead to deformities of the hands (AIHW 2005).
- Osteoporosis is a condition whereby there is a progressive loss of bone density and decrease in the strength of the skeleton with a resultant risk of fracture (AIHW 2005).
- Chronic back pain can be attributed to numerous causes including muscle strain or the displacement of an intervertebral disc (AIHW 2004).
PREVALENCE
- In 2004–05, 31% (6 million) of the population (33% of females and 29% of males) reported having a long-term disease of the musculoskeletal system and connective tissue.
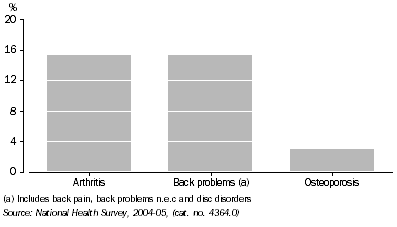
- Of the total population in 2004-05, 15% reported having arthritis, 15% reported having back problems, and 3% reported having osteoporosis.
- In 2004-05, of those with arthritis, 51% reported having osteoarthritis and 16% reported having rheumatoid arthritis.
Prevalence of musculoskeletal conditions, 2004-05
AGE AND SEX
- In 2004–05, the reported prevalence of arthritis was higher for females (18%) than for males (13%).
- Arthritis is a condition most prevalent in older Australians, affecting 49% of people aged 65 years and over in 2004–05 (ABS 2006b).
- The prevalence of back problems was slightly higher for males (16%) than for females (15%).
- Osteoporosis was reported by a higher proportion of females (5%) than males (1%).
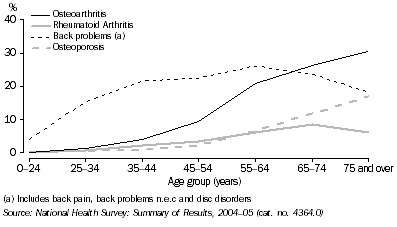
- In 2004-05, osteoarthritis increased with age, being reported by 26% of persons aged 65–74 years and 31% of persons aged 75 years and over.
- The prevalence of rheumatoid arthritis increased with age. In the 65-74 year age group 9% of persons reported the condition, and 6% of persons aged 75 years and over. This compared to 2% of people aged less than 64 years.
- The prevalence of osteoporosis also increased with age, with 12% of persons aged 65–74 years and 17% of persons aged 75 years and over reporting the condition in 2004–05. A higher proportion of females reported osteoporosis in older age groups with 12% of females aged 65-74 years reporting the condition and 26% of females aged 75 and over.
- In contrast, back problems were reported in 24% of persons in the 65-75 year age group in 2004–05. Prevalence of back problems then declined with age with 18% of persons aged 75 years and over reporting the condition.
Musculoskeletal conditions by age, 2004-05
SOCIOECONOMIC STATUS
- In 2004–05, persons aged 15 years and over living in the most disadvantaged areas were more likely to report arthritis (22%) than those living in the least disadvantaged areas (16%); as measured as being in the first and fifth quintiles of the Index of Relative Socio-Economic Disadvantage respectively.
- A similar pattern appears for arthritis when examined by broad age group. Of people in the 15-64 year age group, 16% of those living in the most disadvantaged areas reported arthritis compared to 12% than those living in the least disadvantaged areas. Corresponding figures for those aged 65 years and over were 54% and 49% respectively.
- Similarly, people aged 15 years and over living in the most disadvantaged areas were more likely to report suffering from back problems (21%) than those living in the least disadvantaged areas (17%).
INDIGENOUS AUSTRALIANS
- After adjusting for age differences, a slightly higher proportion of Indigenous Australians reported having a disease of the musculoskeletal system and connective tissue than non-Indigenous Australians in 2004-05 (33% and 30% respectively) (ABS 2006a).
- Indigenous Australians were slightly more likely to report having arthritis than non-Indigenous Australians (18% compared to 15%) and back problems (18% compared to 16%), after adjusting for age differences (footnote 1). The proportion of Indigenous Australians reporting osteoporosis was similar to that for non-Indigenous Australians (2% compared to 3%) (ABS 2006a).
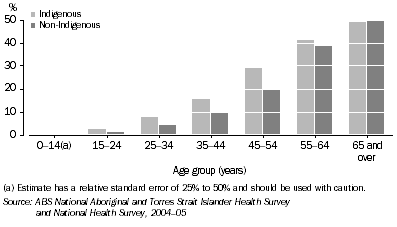
- Arthritis is a condition most prevalent in older Australians, affecting 49% of both Indigenous and non-Indigenous people aged 65 years and over in 2004–05 (ABS 2006b).
- Although similar rates of arthritis were reported for older Indigenous and non-Indigenous Australians in 2004–05, in younger age groups arthritis was more prevalent among Indigenous people (ABS 2006b).
Prevalence of arthritis by Indigenous status, 2004-05
DISABILITY
- According to the 2003 Survey of Disability, Ageing and Carers (SDAC) (footnote 2), 6.8% of the whole population had a disability related to diseases of the musculoskeletal system or connective tissue as the main underlying condition, more than any other medical condition (ABS 2004).
- This equates to 34% of all people with a disability (ABS 2004). The rate is similar across the broad age groups, being 33% for people 0-64 years of age and 34% for those aged 65 years and over.
- Nearly one third of those persons reporting a disease of the musculoskeletal system or connective tissue as the main underlying condition (28%) had either a profound or severe core activity limitation in mobility, self care or communication (ABS 2004).
HEALTH STATUS
- A large proportion of those who reported suffering from some form of arthritis as a long term condition also reported suffering other conditions: 30% reported having hypertension; 19% reported high cholesterol levels; 18% reported suffering chronic lower respiratory diseases and 16% reported having long term mental and behavioural problems.
- Of those persons over 15 years of age who reported suffering from some form of arthritis, 8.8% reported their self-assessed health status as excellent, 25% reported it as very good, 31% reported it as good, 23% reported it as fair, and 12% reported it as poor.
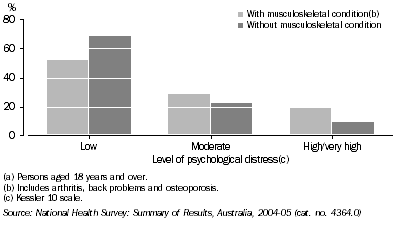
- Using the Kessler Psychological Distress Scale (K10) (footnote 3), adults with a musculoskeletal condition reported higher levels of psychological distress. In 2004–05, of those without arthritis, back problems, or osteoporosis, 68% had a low level of psychological distress, 22% had a moderate level, and 10% had a high/very high level of psychological distress (after adjusting for age differences). In comparison, those suffering from arthritis, back problems or osteoporosis had lower levels of low psychological distress (52%), slightly higher levels of moderate psychological distress (28%), and higher levels of high/very high psychological distress (20%) (after adjusting for age differences).
Level of psychological distress (a), 2004-05
RISK FACTORS
- A variety of risk factors contribute to the development and progression of arthritis and osteoporosis.
- The risk factors associated with the development of rheumatoid arthritis are largely genetic. However, the presence of high-risk genes is not sufficient to develop the condition. A variety of environmental factors are considered to expose this susceptibility. Something must occur to trigger the onset of the disease such as contracting an infectious virus or bacteria (AIHW 2005).
- The development of osteoarthritis can be attributed to a range of predisposing, biomedical and behavioural risk factors. Predisposing factors include age, sex and genetics. Osteoarthritis may begin at any age, but usually affects older people. Females are at a higher risk of developing the condition, particularly after menopause. Biomedical and behavioural factors include obesity, joint trauma and injury, repetitive occupational use and physical inactivity (AIHW 2005).
- A range of biomedical, genetic, and behavioural risk factors contribute to the development of osteoporosis. Biomedical and genetic factors include age, being post-menopausal, low body weight, poor vitamin D status, and family history. Behavioural risk factors include low calcium intake, smoking, physical inactivity and excessive alcohol consumption (AIHW 2005). Other medical conditions, physical disabilities, and a previous history of bone fractures are also risk factors for the development of osteoporosis (AIHW 2005).
Long-Term Injuries
- In the 2004–05 NHS, musculoskeletal conditions were the most commonly reported long-term condition due to an injury. Musculoskeletal conditions accounted for a quarter (25%) of all long-term conditions due to injury; 31% of those with back problems; 16% of those with rheumatism and other soft tissue disorders; and 12% of those with arthritis reported the condition was due to an injury (ABS 2006c).
Physical Inactivity
- Physical inactivity has been identified as a behavioural risk factor for osteoarthritis, and has also been identified as a risk factor for osteoporosis, particularly during growth and adolescence. Appropriate levels of physical activity and weight bearing activities can slow bone mineral loss, and maintain bone mass (AIHW 2005). Gentle, regular exercise can improve an arthritic joint by nourishing the cartilage and easing stiffness (DHS 2006).
- Persons aged 15 years and over with osteoarthritis in 2004–05 were more likely to report being sedentary (37%) than those without the condition (33%) (after adjusting for age differences). However, a similar proportion of those with osteoarthritis reported a low level of exercise (35%) compared to those without the condition (36%).
- In 2004–05, persons aged 15 years and over with osteoporosis were as likely to be sedentary (32%) as those without osteoporosis (33%) (after adjusting for age differences). However, those with osteoporosis were more likely to report a low level of exercise (44%) compared to those without the condition (36%).
Overweight and Obesity
- Obesity has been identified as a behavioural risk factor for osteoarthritis (AIHW 2005).
- In 2004–05, 65% of persons aged 15 years and over who reported osteoarthritis (and their height and weight) were classified as overweight/obese, compared to 53% of those without osteoarthritis (after adjusting for age differences).
ACTIONS TAKEN FOR ARTHRITIS/OSTEOPOROSIS
- More than half (59%) of persons with arthritis and/or osteoporosis reported that they took some action for the condition in the fortnight preceding the time of interview for the 2004-05 NHS.
- Pharmaceutical medications were used by 37% of people reporting these conditions, while 40% used vitamins, minerals or herbal treatments (ABS 2006c).
- Females (48%) were more likely than males (29%) to use vitamins, minerals or herbal treatments for arthritis or osteoporosis (ABS 2006c).
- Lifestyle changes were also common among people with arthritis or osteoporosis, with 18% reporting they exercised most days, 6% did weights/strength/resistance training and 6% used massage as a treatment. Also, 10% consulted a general practitioner or specialist and 4% visited another health professional (ABS 2006c).
HEALTH SYSTEM COSTS
- Arthritis and other musculoskeletal conditions accounted for 3.5% of all hospital separations (as principle diagnosis) in public hospitals, and 8.3% of all hospital separations (as principle diagnosis) in private hospitals in 2003-04 (AIHW 2006).
- In 2000-01, 9.2% of total allocated health expenditure ($4.6 billion) was spent on musculoskeletal conditions, only less than cardiovascular diseases (10.9%) and diseases of the nervous system (9.9%) (AIHW 2005).
- Of the total expenditure on musculoskeletal conditions in 2000-01, osteoarthritis accounted for one-quarter ($1.2 billion) of the expenditure, chronic back pain accounted for 12% ($567 million), slipped disc accounted for 6% ($299 million), and rheumatoid arthritis and osteoporosis both accounted for 5% each ($246 million and $221 million respectively) (AIHW 2005).
- Out-of-hospital medical services for arthritis and musculoskeletal conditions cost $879 million in 2000-01, accounting for 19% of the total expenditure for musculoskeletal conditions. This was the largest amount spent (proportionately) on any disease group in Australian in 2000-01 for out-of hospital medical services (AIHW 2005).
- Hospital costs contributed 39% to the total health system costs on musculoskeletal conditions in 2000-01 (AIHW 2005).
- The greatest proportion of expenditure incurred for osteoarthritis was for hospital services (48%). More than 87% of this expenditure was admitted patient costs (AIHW 2005).
- The largest component of expenditure for rheumatoid arthritis was for hospital services (28%). Almost two-thirds of this expenditure was spent on non-admitted patient services (AIHW 2005).
- The greatest proportion of expenditure for osteoporosis was on pharmaceutical treatment (35%). Prescription medications comprised 97% of this expenditure (AIHW 2005).
MORTALITY
- Arthritis and other musculoskeletal conditions account for a small percentage of deaths (AIHW 2004).
- In less than 1% of deaths registered in 2004, diseases of the musculoskeletal system were reported as the underlying cause of death and in a further 3% of deaths, diseases of the musculoskeletal system were reported as a contributing or associated cause of death (ABS 2006).
FOOTNOTES
1. Since many health characteristics are age-related, the age profile of the populations being compared needs to be considered when interpreting the data. To account for the differences in age structure, much of the comparative data contained within this publication are shown as age standardised percentages. For further detail, see the Explanatory Notes of the National Health Survey: Summary of Results, 2004–05 (cat. no. 4364.0). Back
2. The 2003 Survey of Disability, Ageing and Carers (SDAC) included people in both private and non-private dwellings, including people in cared accommodation establishments but excluding those in gaols and correctional institutions (ABS 2004). The survey aimed to collect information about three population groups: people with a disability, older people (i.e. those aged 60 years and over), and people who provide assistance to older people and people with disabilities (ABS 2004). Back
3. The Kessler Psychological Distress Scale - 10 (K10) is used as a measure of non-specific psychological distress. A very high level of psychological distress, as shown by the K10, may indicate a need for professional help. In the 2004-05 NHS, the K10 questions were asked of adults aged 18 years and over. For more information, see Australian Bureau of Statistics Information Paper: Use of Kessler Psychological Distress Scale in ABS Health Surveys, 2003 (cat. no. 4817.0.55.001). Back
LIST OF REFERENCES
Australian Bureau of Statistics 2006, Causes of Death Australia, 2004, cat. no. 3303.0, ABS, Canberra.
Australian Bureau of Statistics 2006a, National Aboriginal and Torres Strait Islander Health Survey, 2004–05, cat. no. 4715.0, ABS, Canberra.
Australian Bureau of Statistics 2006b, National Aboriginal and Torres Strait Islander Health Survey, 2004–05, unpublished data.
Australian Bureau of Statistics 2006c, National Health Survey: Summary of Results, Australia, 2004–05, cat. no. 4364.0, ABS, Canberra.
Australian Bureau of Statistics 2004, Disability, Ageing and Carers: Summary of Findings, Australia, 2003, cat. no. 4430.0, ABS, Canberra.
Australian Institute of Health and Welfare 2006, Australia's Health, AIHW Cat No. AUS 73, AIHW, Canberra.
Australian Institute of Health and Welfare 2005, Arthritis and musculoskeletal conditions in Australia, 2005, AIHW Cat. No. PHE67, AIHW, Canberra.
Australian Institute of Health and Welfare 2004, Australia's Health, AIHW Cat. No. AUS 44, AIHW, Canberra.
Department of Human Services, Victoria, Better Health Channel 2006, Arthritis and Water Exercise, viewed June 2006,
www.betterhealth.vic.gov.au/bhcv2/bhcarticles.nsf/pages/Arthritis_and_water_exercise?OpenDocument
|
|
 Print Page
Print Page
 Print All
Print All